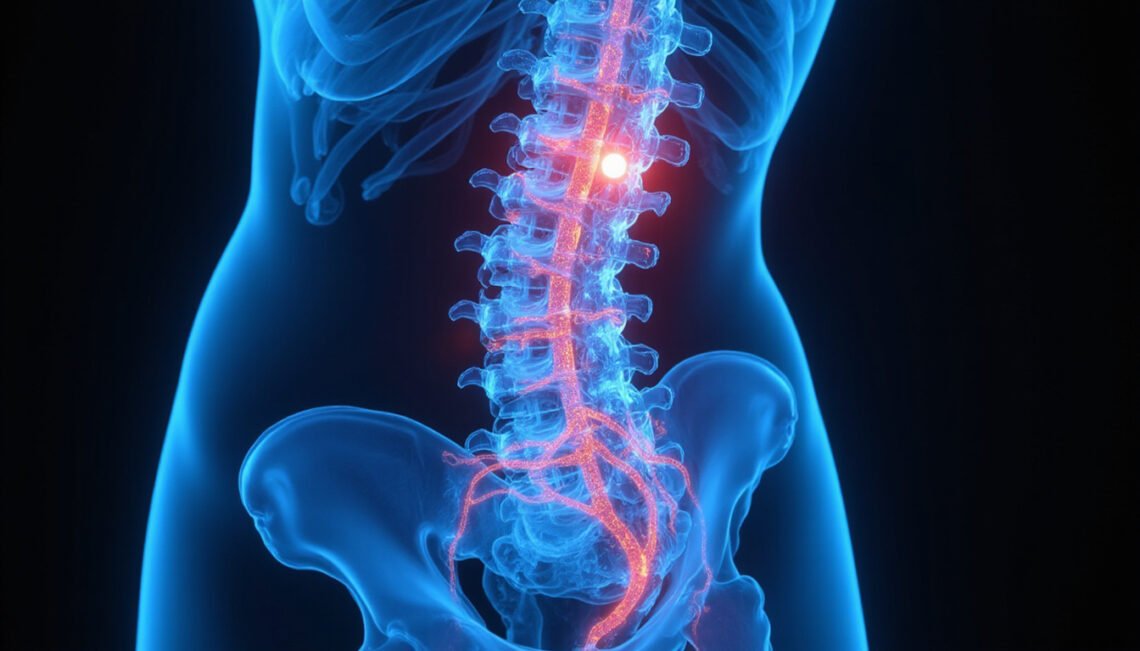
For many people living with stubborn low back, pelvic, or leg pain, the real culprit may be something they’ve never heard of: a Tarlov cyst. Often dismissed as an “incidental finding” on MRI scans, these fluid-filled sacs near the spinal nerve roots can, in some cases, cause significant pain and neurological symptoms. Because they’re frequently misunderstood or overlooked, many patients spend years searching for answers.
This guide explains what Tarlov cysts are, why they can cause chronic pain, how they’re diagnosed, and what treatment options exist—from conservative care to specialized surgical procedures.
What is a Tarlov cyst?
A Tarlov cyst, also called a perineural or sacral nerve root cyst, is a fluid-filled sac that forms around the nerve roots at the base of the spine, most often in the sacrum (the triangular bone just above the tailbone).
Key features:
- Filled with cerebrospinal fluid (CSF), the same fluid that cushions the brain and spinal cord
- Usually located in the sacral region (S1–S4) around the dorsal nerve root
- Can be single or multiple and vary greatly in size
- Many are small and asymptomatic; a subset become symptomatic and painful
Though they are relatively uncommon in the general population, Tarlov cysts appear in about 4–9% of people who undergo lumbosacral MRI imaging (source: National Center for Biotechnology Information ). Only a fraction of those individuals, however, will develop symptoms.
Why Tarlov cysts are often missed or minimized
Despite being visible on imaging, a Tarlov cyst is frequently downplayed or ignored as a cause of pain. There are several reasons for this:
-
Historically considered “incidental”
For many years, radiologists and clinicians were taught these cysts seldom cause symptoms. As a result, they were often glossed over in MRI reports. -
Symptoms mimic other spine conditions
Tarlov cyst–related pain can resemble sciatica, disc herniation, sacroiliac joint dysfunction, or pelvic floor disorders, making diagnosis challenging. -
Lack of widespread clinical familiarity
Many clinicians rarely see symptomatic cases and may not know how to correlate cyst size, location, and imaging findings with the patient’s symptoms. -
Variable correlation between size and symptoms
Some patients with big cysts have minimal discomfort; others with smaller cysts can experience severe pain. This inconsistency adds to clinical uncertainty.
Because of this, patients may be told their imaging is “normal” or their cyst is “too small to cause issues,” even when their pain pattern and neurological signs strongly suggest otherwise.
Symptoms and warning signs of a symptomatic Tarlov cyst
Many people with a Tarlov cyst never develop symptoms. When cysts do become symptomatic, it’s usually because they compress or irritate nearby nerve roots, erode bone, or disrupt normal cerebrospinal fluid dynamics.
Common symptoms include:
-
Low back or sacral pain
Often deep, aching, or burning, located in the lower back, buttocks, or tailbone region. -
Leg pain (radicular pain)
Shooting, electric, or burning pain that radiates down the buttock, thigh, calf, or foot, similar to sciatica. -
Numbness, tingling, or weakness
Especially in the legs, feet, or around the saddle region (inner thighs, perineum). -
Pelvic and perineal pain
Discomfort in the groin, rectal, or vaginal area; sometimes associated with painful sitting or sexual dysfunction. -
Bladder or bowel changes
Urinary urgency, frequency, incontinence, difficulty starting urination, constipation, or bowel incontinence in more severe cases. -
Worsening with certain positions
Symptoms may increase with sitting, standing, walking, Valsalva maneuvers (coughing, straining), or prolonged activity, and improve when lying down.
Red-flag features that require prompt medical attention include:
- Progressive leg weakness
- New or worsening bowel or bladder incontinence
- Numbness in the saddle area
- Rapid escalation of pain or neurological symptoms
These signs could indicate serious nerve compression and demand urgent evaluation.
What causes a Tarlov cyst?
The exact cause of Tarlov cysts is not fully understood, and likely involves a mix of structural and pressure-related factors.
Possible contributors include:
-
Congenital connective tissue weakness
Some people may be born with weaker dura (the outer covering of the spinal cord and nerves), predisposing them to CSF outpouchings. -
Increased spinal fluid pressure
Elevated cerebrospinal fluid pressure can gradually push the dura outward, forming a cyst around nerve roots. -
Trauma or injury
Falls, car accidents, spinal surgery, or childbirth–related strain may trigger cyst formation or enlargement in susceptible individuals. -
Degenerative spine changes
Age-related changes might alter pressure dynamics and contribute to cyst growth. -
Connective tissue disorders
Conditions such as Ehlers–Danlos syndrome or Marfan syndrome may increase vulnerability, though not all patients have these conditions.
In many cases, no single cause is identified; instead, several risk factors likely converge over time.
How a Tarlov cyst is diagnosed
Diagnosis involves correlating clinical symptoms with imaging findings and ruling out other possible causes.
1. Detailed medical history and physical exam
A clinician will ask about:
- Location, character, and timing of pain
- Aggravating and relieving factors (e.g., sitting vs. lying)
- Neurological symptoms (numbness, tingling, weakness)
- Bladder, bowel, or sexual function changes
- Past injuries, surgeries, or underlying conditions
A focused neurological exam looks for:
- Reflex changes
- Muscle strength deficits
- Sensory loss along specific nerve distributions
- Gait abnormalities
2. Imaging studies
-
MRI (Magnetic Resonance Imaging)
The primary tool to detect a Tarlov cyst. MRI shows cyst size, number, and relationship to nerve roots and surrounding bone. -
CT scan or CT myelogram
May be used to evaluate bone erosion or confirm communication with the subarachnoid space (where CSF circulates). -
X-rays
Less useful for cysts themselves, but can show sacral bone changes or other spinal problems.
3. Correlation and differential diagnosis
Finding a Tarlov cyst on MRI does not automatically mean it is the pain source. Clinicians must:
- Match symptoms to affected nerve roots
- Exclude other conditions (disc herniation, spinal stenosis, sacroiliac joint issues, peripheral neuropathy)
- Sometimes use diagnostic injections (e.g., nerve blocks) to see if pain improves when a suspected nerve is numbed
Accurate diagnosis often benefits from input by a spine specialist, neurosurgeon, or neurologist familiar with Tarlov cysts.
Treatment options for a Tarlov cyst
Not every Tarlov cyst needs treatment. Management depends on:
- Symptom severity
- Impact on daily function and quality of life
- Evidence of nerve damage or progressive deficits
- Cyst size, location, and structural effects (e.g., bone erosion)
Treatments typically fall into three categories: conservative, interventional, and surgical.
Conservative (non-surgical) management
For mild to moderate symptoms or when surgery poses high risk, conservative care is often the first step:
-
Medications
- NSAIDs (ibuprofen, naproxen) for mild pain and inflammation
- Neuropathic pain agents like gabapentin, pregabalin, or certain antidepressants (e.g., duloxetine)
- Short-term use of stronger pain medications if required and closely monitored
-
Physical therapy
Gentle programs focused on:- Core strengthening and postural alignment
- Flexibility and nerve-gliding techniques
- Activity modification to reduce nerve irritation
-
Lifestyle and ergonomic changes
- Limiting prolonged sitting; using a standing desk or frequent breaks
- Cushions or donut pillows to reduce sacral pressure
- Avoiding heavy lifting and high-impact activities that worsen symptoms
-
Pelvic floor therapy
For patients with pelvic pain, urinary, or sexual dysfunction, specialized pelvic floor rehabilitation can provide meaningful relief.
Conservative care may not eliminate symptoms, but can significantly improve function and comfort for some patients.
Interventional procedures
If symptoms persist despite conservative strategies, minimally invasive interventions may be considered. These are typically performed by interventional radiologists or pain specialists.
Common options:
-
Epidural steroid injections
- Steroid medication is injected near the affected nerve roots to reduce inflammation and pain.
- Results may be temporary but can help manage flares or confirm pain sources.
-
CT-guided aspiration and fibrin glue injection
- Under imaging guidance, the cyst is punctured, CSF is aspirated, and a fibrin glue substance is injected to seal the cyst and prevent refilling.
- Some patients experience substantial pain reduction; others have temporary or minimal benefit.
- There is risk of recurrence and potential complications (CSF leak, infection, nerve irritation).
These procedures are not appropriate for every Tarlov cyst and should be discussed thoroughly with a knowledgeable specialist.
Surgical options for Tarlov cysts
Surgery is generally reserved for:
- Severe, disabling pain unresponsive to other treatments
- Progressive neurological deficits (weakness, loss of sensation)
- Significant bladder or bowel dysfunction
- Large cysts causing bone erosion or structural instability
Because a Tarlov cyst involves nerve roots and the delicate dural sac, surgery is complex and should be performed by a neurosurgeon experienced in this condition.
Common surgical techniques include:
-
Microsurgical fenestration and imbrication
- The cyst wall is opened (fenestrated), drained, and partially removed or folded (imbricated).
- The defect is repaired to prevent CSF re-accumulation.
-
Cyst resection or partial removal
- In select cases, part or all of the cyst wall can be removed without injuring the nerve roots.
-
Decompression and stabilization
- If cysts have eroded bone or caused instability, additional procedures (e.g., fusion) may be necessary.
Potential benefits:
- Reduced pain and improved neurological function
- Decreased pressure on nerves and surrounding structures
Risks and considerations:
- CSF leaks and pseudomeningoceles
- Infection or wound healing complications
- New or worsened nerve symptoms
- Cyst recurrence or incomplete symptom relief
Because outcomes vary, an honest risk–benefit discussion with a surgeon is crucial, and getting a second opinion can be valuable.
Living with a Tarlov cyst: Self-advocacy and coping strategies
For many patients, a Tarlov cyst is a chronic condition that requires ongoing management rather than a one-time fix. Helpful strategies include:
-
Tracking symptoms
Keep a journal noting pain levels, activities, and triggers. This helps refine treatment and communicate clearly with clinicians. -
Optimizing overall health
Adequate sleep, anti-inflammatory nutrition, and stress management can reduce pain sensitivity. -
Gentle movement
Activities like walking, swimming, or low-impact yoga (within comfort) can maintain mobility and reduce stiffness. -
Mental health support
Chronic pain is emotionally draining. Counseling, cognitive-behavioral therapy, or support groups can improve resilience and coping. -
Educating yourself and your care team
Bringing reputable resources to appointments can help ensure your Tarlov cyst is taken seriously and thoughtfully evaluated.
FAQ about Tarlov cysts and chronic pain
1. Can a Tarlov cyst cause sciatica-like pain?
Yes. A sacral Tarlov cyst can compress or irritate the sacral nerve roots, leading to pain that travels down the buttock and leg, similar to sciatica from a lumbar disc herniation. The pattern of symptoms often depends on which specific nerve roots are affected.
2. Do all perineural cysts need surgery?
No. Most perineural (Tarlov) cysts are asymptomatic and do not require treatment. Only a small percentage cause significant pain or neurological deficits. In those cases, treatment usually starts conservatively, and surgery is reserved for severe or progressive cases after careful evaluation.
3. Are sacral nerve root cysts permanent, or can they go away on their own?
Many sacral nerve root cysts remain stable over time. Some may slowly enlarge, while spontaneous complete resolution is rare. Symptoms, however, can fluctuate significantly. With targeted conservative care or interventional procedures, patients often achieve substantial symptom improvement, even if the cyst itself remains visible on imaging.
Take the next step toward answers and relief
If you’ve been living with persistent low back, pelvic, or leg pain and your imaging report mentions a Tarlov cyst, it’s worth a deeper look. These cysts are not always “incidental,” and in some cases, they are a treatable source of chronic pain and neurological symptoms. You don’t have to accept vague explanations or live indefinitely with disabling discomfort.
Speak with a spine specialist, neurosurgeon, or neurologist who has experience evaluating Tarlov cysts. Bring your MRI reports, a detailed symptom history, and any questions you have about conservative, interventional, or surgical options. With the right information and a collaborative care team, you can move closer to an accurate diagnosis and a personalized plan for meaningful relief.