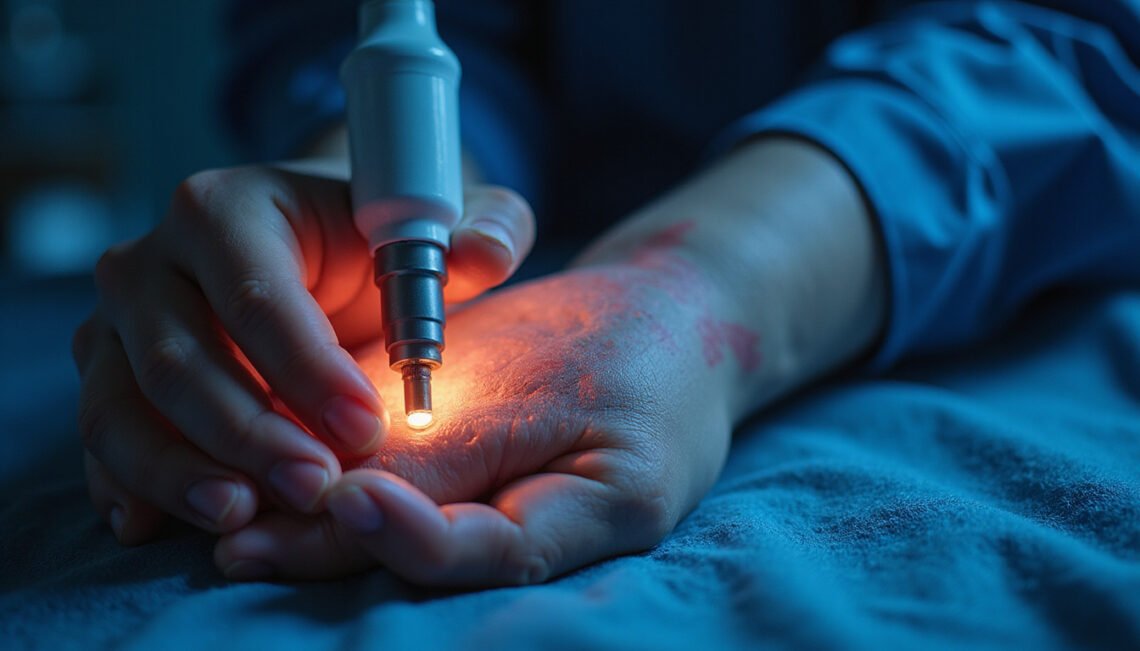
Nerve ultrasound is rapidly changing how doctors diagnose and treat nerve problems. By providing real-time images of nerves, muscles, and surrounding tissues, it helps clinicians see exactly what’s happening under the skin—often faster, more comfortably, and more affordably than traditional imaging. This essential guide explains how nerve ultrasound works, when it’s used, what to expect during the exam, and how it can speed up your path to relief.
What Is Nerve Ultrasound?
Nerve ultrasound, also called neuromuscular or peripheral nerve ultrasound, is a noninvasive imaging test that uses high-frequency sound waves to create detailed pictures of nerves and nearby structures.
Unlike MRI or CT, nerve ultrasound:
- Uses no radiation
- Can be done at the bedside or in the clinic
- Shows nerves moving in real time
- Allows side-by-side comparison of normal and abnormal areas
A specially trained clinician—often a neurologist, physiatrist, radiologist, or sonographer—moves a handheld probe (transducer) over your skin. The machine converts reflected sound waves into images, allowing the examiner to assess the shape, size, continuity, and movement of your nerves.
How Nerve Ultrasound Works in Simple Terms
The technology behind nerve ultrasound is sophisticated, but the basic idea is simple:
- The transducer emits high-frequency sound waves into your tissues.
- Different tissues (skin, fat, nerves, tendons) reflect sound differently.
- The ultrasound machine converts these echoes into grayscale images.
- The clinician interprets the images and may take measurements of nerve size or cross-sectional area.
Healthy nerves have a characteristic “honeycomb” appearance in cross-section. When a nerve is compressed, inflamed, or injured, this pattern can change—often becoming swollen, flattened, or disrupted. These visual changes help pinpoint the cause of your symptoms.
Why Nerve Ultrasound Matters for Faster Diagnosis
Timely diagnosis is critical in nerve disorders. Long-standing compression or injury can result in permanent damage. Nerve ultrasound offers several advantages that can speed up diagnosis and treatment:
- Immediate visualization: Results are available in real time—no waiting days for imaging reports.
- Targeted assessment: Doctors can examine the exact area where you have pain, tingling, or weakness.
- Dynamic testing: Nerves and tendons can be observed while you move, which can reveal problems missed on static scans.
- Better planning: Surgeons and interventional specialists can plan more accurate injections and surgeries.
Research and clinical practice increasingly support nerve ultrasound as a valuable complement to traditional nerve conduction studies and electromyography (EMG) for peripheral nerve disorders (source: American Academy of Neurology).
Common Conditions Diagnosed with Nerve Ultrasound
Nerve ultrasound is especially helpful for conditions where nerves are compressed, irritated, or injured. Some of the most common include:
Carpal Tunnel Syndrome
Carpal tunnel syndrome is one of the best-studied uses of nerve ultrasound. The median nerve can be clearly seen at the wrist, and any swelling or flattening can be measured.
Nerve ultrasound helps to:
- Confirm the diagnosis
- Assess severity
- Rule out other causes of symptoms in the hand and fingers
- Guide steroid injections or surgical planning
Ulnar Nerve Entrapment
The ulnar nerve at the elbow (cubital tunnel) or wrist (Guyon’s canal) can be visualized to see:
- Compression points
- Instability or “subluxation” of the nerve when the elbow bends
- Scar tissue or anatomical variations
Peripheral Nerve Injuries
After trauma, surgery, or fractures, nerve ultrasound can help determine:
- Whether a nerve is stretched, compressed, or severed
- If scar tissue is forming around the nerve
- The exact location of the injury
This information can guide whether to observe, inject, or operate.
Nerve Tumors and Masses
Benign nerve tumors (like schwannomas or neurofibromas) and cysts can often be identified by nerve ultrasound. It helps determine:
- The origin of a lump (nerve vs tendon vs other tissue)
- Its relationship to neighboring structures
- Whether surgery is likely to be complex
Scapular, Shoulder, and Foot Nerve Issues
Nerve ultrasound is increasingly used to evaluate:
- Entrapment of nerves around the shoulder (e.g., suprascapular nerve)
- Morton’s neuroma in the foot
- Tarsal tunnel syndrome at the ankle
- Nerve involvement in chronic neck or back-related limb pain
Nerve Ultrasound vs MRI and EMG
Nerve disorders are often evaluated with a combination of tests. Understanding how nerve ultrasound compares helps you know what to expect.
Nerve Ultrasound vs MRI
Advantages of nerve ultrasound:
- Faster and more accessible in many clinics
- Less expensive in most healthcare systems
- Allows real-time, dynamic assessment
- Comfortable for patients with claustrophobia or implants that limit MRI
Advantages of MRI:
- Deep structures and spine are visualized better
- Broad overview of muscles, bones, discs, and organs
- Useful when tumors or complex anatomy are suspected
In many cases, nerve ultrasound is used as the first-line tool, with MRI reserved for more complex or inconclusive cases.
Nerve Ultrasound vs EMG and Nerve Conduction Studies
EMG and nerve conduction studies (NCS) test how well nerves are working, while nerve ultrasound shows what nerves look like.
- EMG/NCS can detect slowed conduction, denervation, or nerve dysfunction, even when anatomy appears normal.
- Nerve ultrasound can show structural problems (compression, swelling, tumors) that explain abnormal test results or point to the precise site of damage.
Often, combining EMG/NCS with nerve ultrasound provides a more complete picture: function plus structure.
What to Expect During a Nerve Ultrasound Exam
If your provider orders a nerve ultrasound, the process is usually simple and quick.
Before the Exam
- Wear loose, comfortable clothing that allows access to the area being scanned.
- You can eat and drink normally—no special preparation is needed.
- Bring a list of your symptoms and where you feel them most strongly.
During the Exam
A typical nerve ultrasound exam involves:
- Positioning: You’ll sit or lie down so the area of interest is accessible and comfortable.
- Gel application: A warm or room-temperature gel is placed on your skin to help the transducer glide smoothly and improve image quality.
- Scanning: The clinician moves the transducer over your skin, sometimes asking you to move (bend your wrist, flex your elbow, wiggle your toes) while watching the nerve in real time.
- Measurements: They may freeze images, record short video clips, and measure nerve size and shape.
- Discussion: In many practices, the clinician will share initial impressions with you immediately.
Most exams last between 15 and 45 minutes, depending on how many areas are studied.
After the Exam
- There is no downtime; you can return to normal activities right away.
- The findings may be used to adjust your treatment plan immediately—such as deciding on splinting, injections, therapy, or surgery.
- A formal report is typically added to your medical record and shared with your referring provider.
Benefits and Limitations of Nerve Ultrasound
Like any medical test, nerve ultrasound has strengths and weaknesses.
Key Benefits
- Noninvasive and safe: No needles, no radiation, and no known long-term risks.
- Patient-friendly: Usually painless and well-tolerated.
- Cost-effective: Typically less costly than MRI, which can be important if you have high deductibles or limited coverage.
- Real-time guidance: Ideal for guiding injections and minimally invasive procedures.
Limitations
- Operator-dependent: Image quality and interpretation depend heavily on the examiner’s experience and training.
- Depth limitations: Deep nerves (especially in the spine or pelvis) can be harder to visualize.
- Not a stand-alone test: May need to be combined with EMG/NCS or MRI to fully understand complex problems.
If nerve ultrasound is recommended, ask whether your provider has specific training and experience in peripheral nerve imaging.
How Nerve Ultrasound Guides Treatment
The goal of nerve ultrasound is not just to diagnose but to enable faster, more precise treatment.
Conservative Management
When nerve ultrasound reveals mild compression or irritation, your doctor may recommend:
- Activity modification or ergonomic changes
- Splints or braces (e.g., night splinting for carpal tunnel)
- Anti-inflammatory medications
- Physical or occupational therapy
Clear imaging can help focus therapy on the true source of the problem.
Image-Guided Injections
Nerve ultrasound is often used to guide:
- Corticosteroid injections for carpal tunnel, Morton’s neuroma, or other entrapments
- Hydrodissection (injecting fluid around a nerve to release adhesions)
- Diagnostic nerve blocks to confirm the source of pain
Using ultrasound guidance improves accuracy and may reduce the risk of complications compared with “blind” injections.
Surgical Planning and Follow-Up
For patients who need surgery, nerve ultrasound can:
- Identify the exact compression site to plan smaller, targeted incisions
- Reveal anatomical variants that may change the surgical approach
- Check healing and detect recurrent compression or scar-related problems after surgery
This precision can shorten operating times and potentially improve outcomes.
When Should You Ask About Nerve Ultrasound?
Consider discussing nerve ultrasound with your healthcare provider if:
- You have numbness, tingling, or burning pain that follows a nerve distribution and hasn’t improved with basic measures.
- You’ve been told you have carpal tunnel syndrome or another entrapment but want clearer confirmation before surgery.
- You’ve had trauma or surgery and now have persistent nerve symptoms.
- Previous tests (like EMG or MRI) were inconclusive, or your symptoms don’t match earlier findings.
Not every patient needs nerve ultrasound, but in the right situations it can reduce guesswork, speed up diagnosis, and clarify the best next step.
FAQ About Nerve Ultrasound and Related Tests
1. Is an ultrasound of nerves as accurate as other nerve imaging?
An ultrasound of nerves can be very accurate for many peripheral nerve problems, especially entrapment syndromes like carpal tunnel. In experienced hands, it often matches or complements MRI for these conditions and adds the benefit of dynamic, real-time assessment. For very deep structures or complex tumors, MRI may still be preferred, so doctors often use both modalities when necessary.
2. What is a neuromuscular ultrasound, and how is it different?
Neuromuscular ultrasound is a broader term that includes nerve ultrasound plus imaging of muscles, tendons, and sometimes blood vessels. It is used to evaluate both nerves and the muscles they control. For example, in suspected nerve damage, neuromuscular ultrasound can show whether the nerve is compressed and whether the muscle has started to atrophy or change due to lack of nerve input.
3. Do I still need EMG if I have a nerve ultrasound scan?
In many situations, yes. A nerve ultrasound scan shows the structure of the nerve but not how well it functions. EMG and nerve conduction studies measure electrical activity and conduction speed, revealing functional problems that may not yet be visible on ultrasound. Combining the two often provides the most complete, accurate diagnosis and helps avoid unnecessary or ineffective treatments.
Take the Next Step Toward Faster Relief
Persistent numbness, tingling, or nerve pain can be frustrating and life-limiting—but you don’t have to wait months for answers. Nerve ultrasound offers a quick, safe, and precise way to see what’s actually happening to your nerves, often right in your doctor’s office. If you’ve been struggling with unclear diagnoses or are facing decisions about injections or surgery, ask your neurologist, physiatrist, or orthopedic surgeon whether nerve ultrasound is appropriate for your condition.
The sooner you get a clear picture of your nerve health, the sooner you and your care team can choose the most effective treatment—and get you back to using your hands, arms, and legs with confidence.