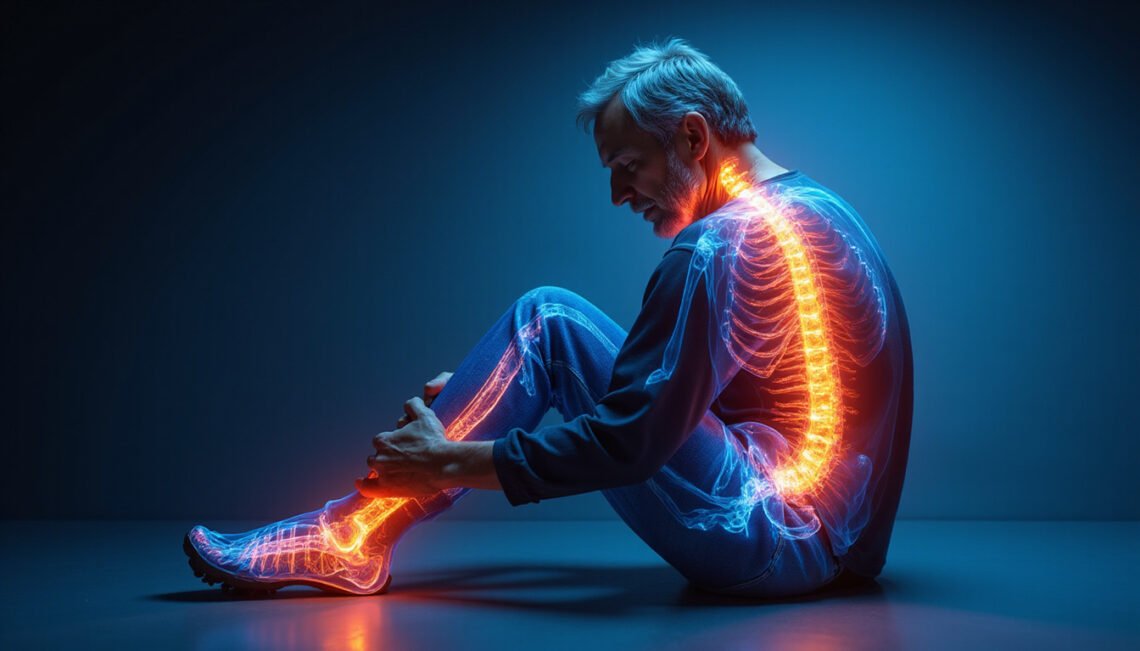
Radiating leg pain can be anything from a mild annoyance to a symptom that stops you in your tracks. Whether it shoots from your lower back down to your foot or burns along the side of your thigh, radiating leg pain often signals an underlying issue with nerves, joints, or blood flow—not just “tired muscles.” Understanding what’s really going on is the fastest way to get relief and prevent long-term damage.
Below, you’ll learn the surprising causes of radiating leg pain, which tests actually help, and the most effective treatment options you can start exploring today.
What Is Radiating Leg Pain, Exactly?
Radiating leg pain is discomfort that starts in one area—often the lower back, hip, or buttock—and travels (or “radiates”) along the course of a nerve into the leg. It may feel:
- Sharp, electric, or shooting
- Burning, tingling, or like “pins and needles”
- Achy, throbbing, or heavy
- Accompanied by numbness or weakness
Key clue: Radiating pain usually follows a line or pattern, often down the back, side, or front of the leg, rather than spreading evenly across the whole limb.
Surprising Causes of Radiating Leg Pain
Most people immediately think “sciatica,” but radiating leg pain has many possible causes. Some are minor and reversible; others need prompt medical attention.
1. Lumbar Disc Problems (More Than Just Sciatica)
The most common cause is irritation or compression of nerve roots in the lower spine:
- Herniated disc – The soft inner part of a spinal disc pushes out and presses on a nerve root.
- Bulging disc – The disc protrudes but may not be fully herniated.
- Degenerative disc disease – Age-related disc wear narrows the space where nerves exit.
This typically causes:
- Pain in the lower back that radiates down the buttock and leg
- Numbness or tingling in a specific area (e.g., outer calf or foot)
- Worsening with bending, sitting, or coughing
Sciatica is the classic example of radiating leg pain from a lumbar nerve root problem.
2. Piriformis Syndrome: The “Fake Sciatica”
The sciatic nerve passes under or through a small muscle deep in your buttock called the piriformis. If this muscle becomes tight, spasmodic, or injured, it can compress the sciatic nerve, causing:
- Buttock pain that radiates down the back of the leg
- Worse with sitting, climbing stairs, or getting out of a car
- Often no significant low back pain
This gets mistaken for spinal sciatica, but the true culprit is in the hip/buttock region.
3. Hip Joint Arthritis and Labral Tears
Hip problems typically cause groin pain, but they can also trigger radiating leg pain:
- Hip osteoarthritis – Cartilage wear causes deep joint pain that may travel to the thigh or knee.
- Labral tear – Damage to the rim of cartilage around the hip socket can cause sharp, catching pain that radiates down the leg.
Clues pointing to the hip:
- Pain is worse with weight-bearing (standing, walking).
- Difficulty putting on shoes or socks due to hip stiffness.
- Pain often felt in the groin or front of the thigh, sometimes down to the knee.
4. Spinal Stenosis: Narrowing of the Nerve Highways
Spinal stenosis is a narrowing of the spinal canal or nerve exit canals, often from arthritis, bone spurs, or disc changes. It can cause:
- Aching, burning, or cramping radiating down both legs
- Worse with standing and walking
- Relief when sitting or bending forward (like leaning on a shopping cart)
This “shopping cart sign” is a classic clue that spinal stenosis may be causing your radiating leg pain.
5. Peripheral Neuropathy: Nerve Damage in the Legs
Not all radiating sensations come from the spine. Peripheral neuropathy is damage to nerves in the legs themselves, often due to:
- Diabetes
- Vitamin B12 deficiency
- Alcohol misuse
- Certain medications (including some chemotherapy drugs)
Typical features:
- Burning, tingling, or numbness in a “stocking” pattern (feet and lower legs)
- Often worse at night
- May affect both legs symmetrically
This may feel like radiating leg pain, but the origin is local nerve damage, not a compressed nerve root.
6. Vascular Problems: When Blood Flow Is the Issue
Sometimes, what feels like nerve pain is actually vascular pain:
- Peripheral artery disease (PAD) – Narrowing of leg arteries causes cramping pain with walking (claudication) that eases with rest.
- Deep vein thrombosis (DVT) – A blood clot in a deep leg vein can cause pain, swelling, and warmth. This is an emergency.
Clues for PAD or DVT:
- One leg suddenly swollen, red, and painful (DVT warning sign).
- Pain that consistently starts after a certain walking distance and resolves with rest (PAD).
If you suspect DVT—especially after surgery, long travel, or immobilization—seek emergency care.
7. Sacroiliac Joint Dysfunction
The sacroiliac (SI) joints connect your spine to your pelvis. When inflamed or misaligned, they can cause:
- Pain near the dimples of your lower back/upper buttocks
- Radiating pain into the buttock, groin, or back of the thigh
- Worse with standing on one leg, climbing stairs, or rolling over in bed
SI joint pain is often overlooked but is a frequent source of radiating leg pain.
8. Less Common but Serious Causes
While rare, serious conditions can cause radiating leg pain:
- Cauda equina syndrome – Massive compression of the lower spinal nerves; causes severe back/leg pain, saddle numbness (inner thighs), and bowel/bladder changes. Emergency.
- Spinal tumors or infections – Unexplained pain, especially with weight loss, fever, or night pain.
- Fractures – After trauma, osteoporosis, or steroid overuse.
Any red-flag symptoms (see below) should be evaluated urgently.
When Radiating Leg Pain Is an Emergency
Seek immediate medical care if radiating leg pain is accompanied by:
- Loss of bowel or bladder control, or difficulty starting urination
- Numbness in the groin or “saddle” area
- Sudden, severe leg weakness or foot drop
- One leg suddenly swollen, red, warm, and painful (possible DVT)
- Fever, chills, and back pain after surgery, injection, or infection
- Recent significant trauma (e.g., fall from height, car accident)
These could indicate conditions needing urgent treatment to protect nerves or prevent complications.
How Doctors Diagnose Radiating Leg Pain
A careful history and physical exam are the foundation. Radiating leg pain often has a recognizable pattern when the right questions and tests are used.
1. Detailed History
Your clinician may ask:
- Where does the pain start and where does it travel?
- What makes it better or worse (sitting, walking, bending, lying flat)?
- Any numbness, tingling, or weakness?
- Recent injuries, surgeries, infections, or weight loss?
- Other medical conditions (diabetes, vascular disease, cancer)?
The pattern of your answers often points strongly toward the cause before any imaging is ordered.
2. Physical and Neurological Exam
Key components include:
- Back and hip range of motion and palpation for tenderness
- Straight leg raise test – Lifting your leg while lying down to see if it reproduces radiating pain (often positive in sciatica).
- Reflexes – At the knee and ankle
- Strength testing – For hip flexion, knee extension, ankle dorsiflexion/plantarflexion
- Sensation testing – Light touch or pinprick along different nerve territories
These tests help pinpoint which nerve or joint might be responsible.
3. Imaging Tests
Imaging is typically ordered if:
- Symptoms last more than 4–6 weeks despite conservative therapy
- There are neurological deficits (weakness, loss of reflexes)
- Red-flag signs suggest something serious
Common tests:
- X-ray – Shows bone alignment, fractures, significant arthritis, and some degrees of spinal degeneration.
- MRI – Best for discs, nerves, ligaments, spinal canal, and soft tissues; often used to confirm suspected disc herniation, stenosis, or tumors.
- CT scan – Useful when MRI isn’t possible or to better visualize bone.
Evidence-based guidelines recommend avoiding routine imaging for simple low back pain with radiating leg pain in the first few weeks unless there are red flags (source: American College of Physicians).
4. Nerve and Blood Flow Studies
Depending on your symptoms, you may also have:
- EMG/NCS (electromyography & nerve conduction studies) – Assess nerve and muscle function; useful for differentiating radiculopathy (nerve root problem) from peripheral neuropathy.
- Doppler ultrasound or ankle-brachial index (ABI) – To evaluate blood flow in the leg arteries when PAD is suspected.
Fast Relief Options for Radiating Leg Pain
Relief depends on the underlying cause, but many strategies can help reduce pain while you work on long-term solutions.
1. Short-Term Self-Care Strategies
For many cases of radiating leg pain from nerve irritation or muscle strain:
- Relative rest – Avoid activities that sharply worsen pain, but don’t stay in bed for days. Gentle movement is better than total rest.
- Cold and heat – Ice packs for 10–15 minutes can reduce acute inflammation; heat can relax tight muscles in the back and buttock.
- Over-the-counter medications –
- NSAIDs (e.g., ibuprofen, naproxen) for pain and inflammation (if safe for you).
- Acetaminophen as an alternative when NSAIDs aren’t appropriate.
Always follow dosage guidelines and consider other medical conditions or medications.
2. Targeted Exercises and Physical Therapy
A physical therapist can be one of your most powerful allies in managing radiating leg pain. Common approaches:
- McKenzie extension exercises for some disc-related pain.
- Core and hip strengthening to support the spine and pelvis.
- Neural mobilization (“nerve glides”) to help irritated nerves move more freely.
- Stretching for tight hamstrings, hip flexors, and piriformis.
Often, consistent exercise over weeks leads to greater pain reduction and improved function than passive treatments alone.
3. Prescription Medications
If over-the-counter options aren’t enough, your clinician may consider:
- Short courses of stronger pain relievers in acute phases.
- Neuropathic pain medications (e.g., gabapentin, pregabalin, certain antidepressants) when nerve pain is prominent.
- Muscle relaxants for severe muscle spasms.
These are typically used short- to medium-term while underlying causes are addressed.
4. Injections and Interventional Procedures
For persistent, severe radiating leg pain:
- Epidural steroid injections – Deliver anti-inflammatory medication near inflamed nerve roots; can provide temporary but sometimes significant relief in conditions like disc herniation or stenosis.
- Facet joint or SI joint injections – Help both diagnose and treat pain from these joints.
- Nerve blocks or radiofrequency ablation – In selected chronic pain cases.
These procedures are usually done under imaging guidance by pain specialists or interventional radiologists.
5. When Surgery Makes Sense
Surgery is reserved for specific situations, such as:
- Persistent, disabling radiating leg pain that hasn’t improved with conservative care over several weeks to months.
- Clear structural cause correlating with symptoms (e.g., large disc herniation, severe spinal stenosis).
- Progressive neurological deficits (worsening weakness, foot drop).
- Emergencies like cauda equina syndrome.
Common procedures include microdiscectomy (removing part of a herniated disc) and laminectomy (widening the spinal canal in stenosis). For appropriately selected patients, these can provide rapid, meaningful relief.
Long-Term Strategies to Prevent Recurrence
To keep radiating leg pain from coming back:
- Maintain a regular exercise routine with core and hip strengthening.
- Use proper lifting mechanics (bend at hips and knees, keep load close).
- Avoid prolonged sitting; take movement breaks every 30–60 minutes.
- Maintain a healthy weight to reduce pressure on the spine and joints.
- Don’t smoke—smoking accelerates disc degeneration and impairs blood flow.
- Manage chronic conditions like diabetes and vascular disease carefully.
Helpful Daily Habits Checklist
Consider integrating these habits into your daily routine:
- 5–10 minutes of core and hip exercises
- Short walk or stretch break every hour of sitting
- Neutral spine posture when working, driving, or using devices
- Regular sleep schedule and stress management practice
- Periodic review of ergonomics at work and home
FAQ About Radiating Leg Pain
1. What causes sharp shooting pain down the leg?
Sharp, shooting radiating leg pain is most often due to nerve irritation or compression, such as a herniated lumbar disc pressing on a nerve root (sciatica), piriformis syndrome, or spinal stenosis. Less commonly, it can be from nerve damage (neuropathy) or even severe joint inflammation. A detailed exam is needed to distinguish among these.
2. How is radiating pain in the leg different from muscle pain?
Muscle pain is usually localized, sore, or crampy and often linked to overuse or strain. Radiating leg pain tends to follow a line or pathway, can feel electric, burning, or tingling, and may be accompanied by numbness or weakness. When pain travels from the back or buttock into the leg, especially below the knee, a nerve-related cause is more likely.
3. Can radiating leg pain go away on its own?
Yes. Many episodes of radiating leg pain—especially from mild disc irritation or muscle-related causes—improve significantly within a few weeks with conservative care like activity modification, gentle exercise, and appropriate medications. However, if pain persists beyond 4–6 weeks, worsens, or is associated with weakness, numbness, or red-flag symptoms, medical evaluation is important to rule out more serious conditions.
If radiating leg pain is interfering with your work, sleep, or daily life, you don’t have to “just live with it.” The earlier you identify the root cause, the sooner you can start the right targeted treatment—and the better your chances of full recovery.
If your symptoms have been lingering or you’re noticing numbness, weakness, or changes in walking, schedule an appointment with a qualified healthcare professional or spine/nerve specialist. Bring a clear description of your radiating leg pain pattern and what aggravates or relieves it. With the right diagnosis and a focused plan, you can move from worrying about every step to walking confidently and comfortably again.