If you’re dealing with a deep ache or sharp pain in your buttock when sitting, running, or bending forward, you might be facing ischial bursitis. This frustrating condition can make simple things—like sitting at your desk, driving, or enjoying a workout—surprisingly painful. The good news: with the right combination of rest, targeted exercises, and medical treatment, most people recover well and get back to normal activity.
This guide walks you through what ischial bursitis is, why it happens, how to relieve the pain quickly, and the best treatment and exercise options to support lasting recovery.
What Is Ischial Bursitis?
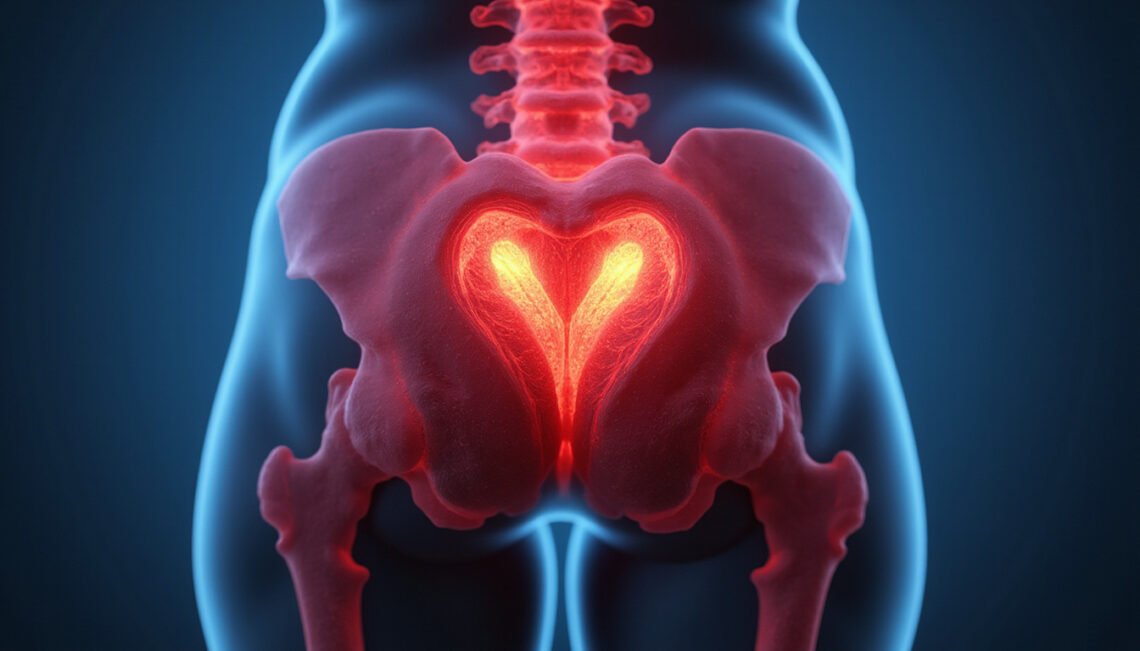
Ischial bursitis (often called “weaver’s bottom”) is inflammation of the bursa over the ischial tuberosity—the bony part you sit on at the bottom of your pelvis.
A bursa is a small, fluid-filled sac that cushions and reduces friction between bones, tendons, and muscles. When the bursa near the ischial tuberosity becomes irritated, it can swell and become painful.
Common Symptoms
People with ischial bursitis typically report:
- Deep ache or burning pain in the lower buttock, right over the “sit bone”
- Pain when sitting, especially on hard surfaces
- Pain that worsens with running, especially uphill, or with hamstring-heavy activities
- Tenderness when pressing on the bony area at the bottom of the buttock
- Stiffness or discomfort when stretching the hamstrings
- Occasional pain radiating down the back of the thigh (often confused with sciatica)
Symptoms can be mild and nagging at first, then progress to sharper pain if not addressed early.
What Causes Ischial Bursitis?
Ischial bursitis is usually caused by repetitive friction or prolonged pressure on the ischial bursa. Common triggers include:
- Prolonged sitting on hard surfaces (e.g., truck drivers, office workers, cyclists, students)
- Running or walking long distances, particularly on hills or uneven terrain
- Sports with repetitive hamstring use, such as sprinting, soccer, and dance
- Direct trauma to the buttock (falling on the buttocks)
- Tight hamstrings or weak glute muscles, which change the load on the pelvis
- Post-surgery or altered gait, leading to compensation patterns
In some cases, systemic inflammatory conditions like rheumatoid arthritis or gout can contribute, but for most active adults, mechanical overuse is the main driver.
Fast Pain Relief for Ischial Bursitis
When the pain flares, your first goal is simply to calm things down. These strategies can provide fast, short-term relief while you address the underlying cause.
1. Modify or Reduce Aggravating Activities
- Limit sitting time, especially on firm chairs or benches.
- Use a cushioned or donut pillow to take pressure off the sit bones.
- Temporarily reduce running, sprinting, and hill workouts.
- Avoid prolonged stretching or aggressive hamstring work during acute flare-ups.
Short, frequent movement breaks (standing, gentle walking) are often better than staying in one position.
2. Ice and Heat
- Ice: For acute or sharp pain, apply an ice pack to the painful area for 10–15 minutes, up to 3 times per day. Always use a cloth between ice and skin.
- Heat: Once the sharpest pain has settled (often after 48–72 hours), you may switch to heat to ease muscle tension—10–15 minutes of a warm pack can relax tight hamstrings and glutes.
Many people find alternating ice and heat helpful; listen to your body and choose what provides more relief.
3. Over-the-Counter Medications
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, can reduce pain and inflammation for short periods.
- Always follow label instructions and speak to your doctor or pharmacist if you have other medical conditions or take regular medications.
Medical Treatment Options for Ischial Bursitis
If home strategies are not enough, or your pain is persistent or severe, a medical professional can guide more targeted treatment.
1. Physical Therapy
A physical therapist will:
- Assess posture, gait, and muscle imbalances
- Use manual therapy and soft-tissue techniques to reduce tension
- Prescribe a progressive exercise plan to restore strength and mobility
- Provide education on ergonomics (how you sit, stand, and move)
This is often the most important long-term treatment for ischial bursitis, not just for relief but for preventing recurrence.
2. Corticosteroid Injections
For severe, stubborn cases, a doctor may recommend an image-guided corticosteroid injection into the inflamed bursa:
- Can provide significant pain relief, especially when pain limits rehab
- Often used alongside physical therapy, not as a stand-alone fix
- Typically limited in frequency due to potential side effects
3. Imaging and Differential Diagnosis
If symptoms don’t improve with conservative care, or if your pain pattern is unusual, your provider may order:
- Ultrasound or MRI to confirm ischial bursitis and rule out:
- Hamstring tendon tear or tendinopathy
- Lumbar disc issues or sciatica
- Hip joint pathology
Correct diagnosis is essential, since sciatica and hamstring injuries can closely mimic ischial bursitis symptoms.
4. Rarely, Surgical Intervention
Surgery to remove the bursa (bursectomy) is rarely required and is usually reserved for:
- Chronic, disabling pain not responding to months of conservative treatment
- Structural abnormalities or associated hamstring tendon damage
Most people never need surgery and respond well to non-surgical management (source: American Academy of Orthopaedic Surgeons).
Best Exercises for Ischial Bursitis Recovery
As pain allows, gentle, progressive exercise is critical to healing. The goals are to:
- Reduce tension in tight muscles
- Strengthen supporting muscles in the hips and core
- Normalize load on the ischial bursa and hamstring tendons
Always move within a pain-free or mildly uncomfortable range (no sharp, stabbing pain). If you’re unsure, consult a physical therapist.

1. Gentle Stretching (Phase 1: When Pain Is Settling)
Start once the worst pain has calmed.
a. Supine Hamstring Stretch (Mild Version)
- Lie on your back with one leg bent, foot on the floor.
- Loop a towel or strap around the other foot.
- Gently straighten the knee until you feel a mild stretch at the back of the thigh—but stop before pain at the sit bone.
- Hold 15–20 seconds; repeat 3–5 times per side.
b. Piriformis / Glute Stretch
- On your back, cross your right ankle over your left knee.
- Gently pull the left thigh toward your chest until you feel a stretch in the right buttock.
- Hold 20–30 seconds; repeat 3–5 times per side.
2. Strengthening the Glutes and Core (Phase 2)
As sitting becomes more comfortable and stretching is tolerated, add strength to offload the ischial area.
a. Glute Bridge
- Lie on your back, knees bent, feet hip-width apart.
- Tighten your core and squeeze your glutes.
- Lift your hips until your shoulders, hips, and knees form a straight line.
- Hold 2–3 seconds, then slowly lower.
- Aim for 2–3 sets of 10–15 reps, once daily.
b. Clamshells
- Lie on your side, knees bent, hips stacked.
- Keep feet together, lift the top knee without rolling your pelvis backward.
- Slowly lower; you should feel this in the side of your hip.
- 2–3 sets of 10–15 reps per side.
c. Side-Lying Leg Raises
- Lie on your side with legs straight.
- Lift the top leg 12–18 inches, keeping it in line with your body.
- Hold briefly, then lower with control.
- 2–3 sets of 10–15 reps per side.
3. Functional and Hamstring Strengthening (Phase 3)
Once basic strength exercises are easy and pain is minimal:
a. Supported Romanian Deadlift (Very Light)
- Stand tall, lightly hold onto a chair or wall for balance.
- Keeping a straight back, hinge at the hips, allowing a slight knee bend.
- Lower your torso until you feel a mild stretch in hamstrings (no sharp pain).
- Use your glutes and hamstrings to return to standing.
- Start with body weight only; 2–3 sets of 8–10 reps.
b. Step-Ups
- Use a low step.
- Step up with one foot, pressing through the heel, then bring the other foot up.
- Slowly step back down.
- 2–3 sets of 10 reps each leg.
If any exercise significantly increases pain at the sit bone during or after, scale back and consult a professional.
Everyday Modifications to Speed Healing
Small daily changes can make a big difference in ischial bursitis recovery.
- Upgrade your seating: Use foam or gel cushions; avoid very firm chairs where possible.
- Alternate positions: Switch between sitting, standing, and light walking.
- Improve posture: Avoid slumping and sitting with your pelvis tipped backward.
- Warm up before exercise: 5–10 minutes of brisk walking or light dynamic stretches.
- Gradual return to running or sports: Follow a structured, step-by-step increase in mileage or intensity.
When to See a Doctor About Ischial Bursitis
See a healthcare professional promptly if you notice:
- Severe, sudden pain or inability to bear weight
- Significant swelling, redness, or warmth at the buttock
- Fever or feeling unwell alongside buttock pain
- Numbness, tingling, or weakness in the leg
- Pain that doesn’t improve after 2–3 weeks of rest and home care
These signs may indicate a different or more serious condition that needs prompt evaluation.
Quick Summary: Managing Ischial Bursitis
To put it all together, effective management of ischial bursitis typically includes:
- Reduce irritation: Modify sitting, use cushions, and ease back on aggravating activities.
- Calm inflammation: Use ice/heat and short-term NSAIDs if appropriate.
- Rehab properly: Commit to targeted stretching and strengthening exercises.
- Seek guidance: Work with a physical therapist or medical provider if symptoms persist.
- Prevent recurrence: Maintain hip and core strength, and avoid long periods of unbroken sitting.
FAQ About Ischial Bursitis
1. How long does ischial bursitis take to heal?
Mild cases of ischial bursitis can improve within 2–4 weeks with rest, activity modification, and basic exercises. More persistent or chronic cases may take 6–12 weeks or longer, especially if muscle imbalances or training errors need to be corrected. Sticking to a consistent rehab plan is the key factor in recovery time.
2. What’s the difference between ischial bursitis vs sciatica?
Though both can cause buttock and back-of-thigh pain, they’re different conditions. Ischial bursitis is inflammation of a bursa over the sit bone and is usually painful when sitting or pressing on that specific spot. Sciatica is irritation or compression of the sciatic nerve, often causing burning, tingling, or numbness running from the low back into the leg and sometimes the foot. A clinician can help distinguish between them through exam and, if needed, imaging.
3. Can I keep running with ischial bursitis?
It depends on pain severity. If running causes sharp pain, alters your gait, or worsens symptoms afterward, it’s best to reduce or pause running and substitute low-impact activities (like cycling with good padding, swimming, or elliptical). As your ischial bursitis improves with treatment and exercises, you can gradually reintroduce running with a structured return-to-run plan guided by a physical therapist or sports medicine professional.
If ischial bursitis is disrupting your work, workouts, or daily life, you don’t have to simply “live with it.” Start today by adjusting your sitting setup, easing off aggravating activities, and adding a few of the gentle stretches and strength moves above. Then, connect with a qualified physical therapist or sports medicine provider who can design a personalized program to get you comfortably back to the activities you love—without that nagging sit-bone pain holding you back.