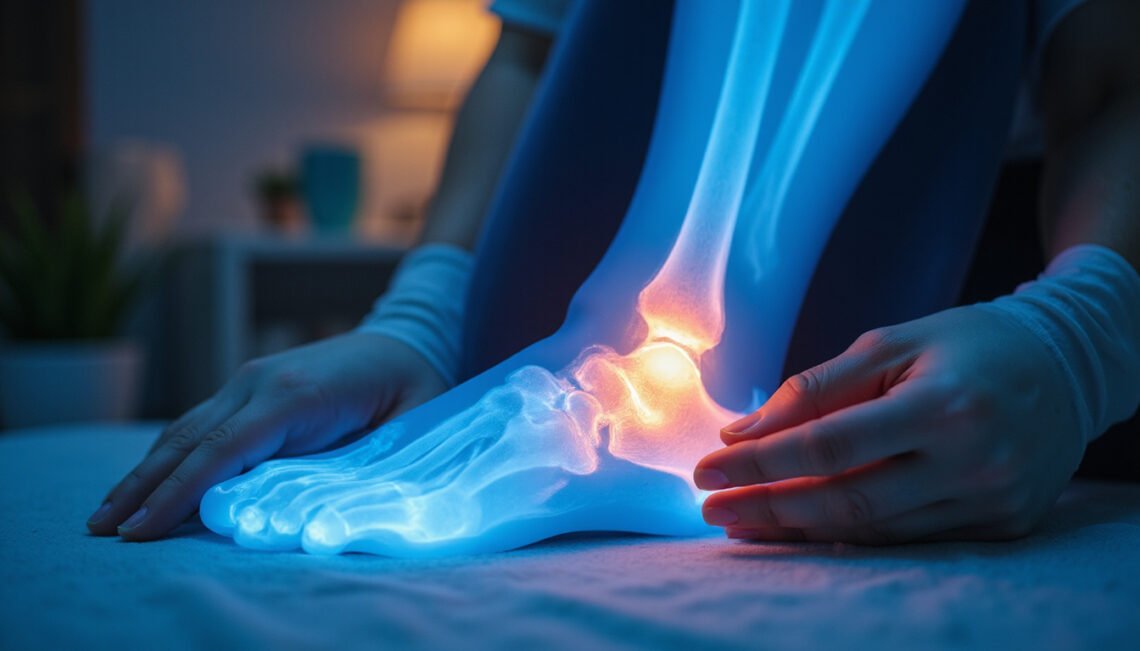
Living with a bone spur can turn simple movements into sharp, nagging pain. Whether it’s in your heel, shoulder, neck, or spine, a bone spur often makes walking, sleeping, and even getting dressed uncomfortable. The good news: bone spur pain doesn’t always require surgery. There are several surprisingly effective treatments—many of them conservative and non-invasive—that can reduce pain, improve mobility, and help you get back to your normal activities.
Below are nine evidence-informed options that actually work for many people, plus practical tips for making each one more effective.
What is a bone spur, really?
Despite the name, a bone spur (also called an osteophyte) isn’t usually a sharp “spike” of bone. It’s an extra bit of bone that forms along the edges of a joint, often where bone meets tendon, ligament, or cartilage.
Common causes include:
- Osteoarthritis and joint wear-and-tear
- Chronic tendon or ligament irritation (like plantar fasciitis in the heel)
- Poor alignment or biomechanics
- Aging and previous injuries
Many bone spurs cause no symptoms at all. They become a problem when they press on nearby nerves, tendons, or other soft tissues, leading to pain, stiffness, and reduced range of motion.
1. Targeted physical therapy and stretching
One of the most effective non-surgical treatments for bone spur pain is a tailored physical therapy program. While a spur itself is bone and won’t disappear with exercise, the surrounding muscles, tendons, and joints can be retrained to reduce pressure and irritation.
How it helps
- Improves joint alignment and mechanics
- Reduces muscle tension pulling on the affected area
- Increases flexibility, especially around the heel, ankle, shoulder, or spine
- Strengthens stabilizing muscles to offload the irritated joint
For example, with a heel bone spur related to plantar fasciitis, a physical therapist may focus on:
- Stretching the calf and plantar fascia
- Strengthening intrinsic foot muscles
- Gait retraining to reduce impact on the heel
Consistent, guided therapy often reduces pain enough that surgery can be avoided or delayed.
2. Custom orthotics and footwear changes
For bone spurs in the feet—especially heel spurs—foot mechanics matter a lot. Poor arch support, flat feet, high arches, or worn-out shoes can increase stress where the spur is located.
Orthotics and shoe strategies
- Custom orthotics (prescribed by a podiatrist) to support your unique arch shape
- Heel cups or pads to cushion a heel spur and reduce pressure when you stand or walk
- Rocker-bottom shoes to reduce the need for excessive toe bending in big-toe bone spurs
- Wider toe boxes if a bone spur affects toe joints and rubs in tight shoes
Even modest changes—like switching to a more supportive walking shoe—can meaningfully reduce symptoms.
3. Anti-inflammatory medications and topical treatments
Inflammation around a bone spur is often what causes the severe pain, not the bone itself. Reducing that inflammation can bring quick relief.
Medication options (with your provider’s guidance)
- NSAIDs: Over-the-counter nonsteroidal anti-inflammatory drugs like ibuprofen or naproxen can reduce pain and swelling when used short-term.
- Topical NSAIDs: Gels or creams (such as diclofenac gel) can be applied directly to the painful area, helping limit whole-body side effects.
- Topical analgesics: Products with menthol, capsaicin, or lidocaine can temporarily alter pain signaling in the skin and surrounding tissues.
These approaches don’t remove the bone spur, but they create a window of relief so you can move more comfortably and continue rehab exercises.
4. Corticosteroid injections
When bone spur pain is severe and doesn’t respond to oral or topical medications, corticosteroid injections can provide powerful, targeted relief.
How they work
A physician injects a corticosteroid (often mixed with a local anesthetic) near the inflamed tissues around the bone spur. This can:
- Dramatically reduce local inflammation
- Provide pain relief that may last weeks to months
- Help confirm that the painful structure is indeed where the injection is placed
Corticosteroid injections are commonly used for:
- Heel spurs associated with plantar fasciitis
- Shoulder bone spurs irritating rotator cuff tendons
- Spinal bone spurs causing nerve irritation
Because repeated steroid injections can weaken tendons or thin cartilage, they’re usually limited in frequency and combined with other treatments like physical therapy for long-term management.
5. Night splints and bracing
Strategic support—especially while you sleep—can be surprisingly effective for bone spur-related pain, particularly in the heel, ankle, and wrist.
Why splints help
Many tissues tighten overnight. In conditions like plantar fasciitis with heel spurs, the plantar fascia shortens while you sleep, then painfully stretches when you take your first morning steps.
Night splints or braces:
- Keep the foot or joint in a gently stretched position
- Reduce the “first-step” pain in the morning
- Let tissues heal in a more optimal length and position
Bracing can also help for bone spurs in the knee, ankle, or wrist by stabilizing the joint, limiting aggravating movements, and allowing inflamed structures to calm down.
6. Ultrasound-guided physical therapy and modalities
Modern physical therapy often goes beyond stretches and exercises. Certain modalities, especially when guided or targeted, can help reduce bone spur-related inflammation and pain.
Common options include:
- Therapeutic ultrasound: Uses sound waves to generate deep, gentle heating in soft tissues, potentially improving blood flow and healing capacity.
- Low-level laser therapy (LLLT): May reduce inflammation and pain in some musculoskeletal conditions, though evidence is mixed.
- Iontophoresis: A technique to deliver anti-inflammatory medication through the skin using a mild electrical current.
While these treatments don’t reshape the bone spur, they can make the tissue around it healthier and more tolerant of movement, especially when combined with a structured exercise plan.

7. Weight management and activity modification
Bone spurs in weight-bearing joints—like knees, hips, feet, and spine—often worsen when those joints are overloaded. Even modest changes to body weight and activity patterns can deliver real relief.
Why this works
- Less weight on the joint = less pressure on the spur and surrounding inflamed tissues
- Lower mechanical stress can slow down further degeneration
- More comfortable movement encourages you to maintain strength and mobility
Helpful strategies include:
- Switching from high-impact activities (running, jumping) to low-impact workouts (cycling, swimming, elliptical)
- Using walking poles or a cane temporarily to offload painful joints
- Working with a dietitian or physician on a realistic weight-loss plan if needed
According to the CDC, losing just 5–10% of body weight can significantly reduce joint pain in people with knee osteoarthritis (source: CDC).
8. Shockwave therapy (ESWT)
Extracorporeal shockwave therapy (ESWT) is a non-invasive treatment that uses high-energy sound waves directed at the painful area. It’s used most often for chronic plantar fasciitis with a heel bone spur and certain tendon problems.
Potential benefits
- Stimulates local blood flow and metabolic activity
- Promotes tissue healing in chronic conditions
- May reduce nerve sensitivity around the spur
For stubborn heel spur pain that hasn’t responded to stretching, orthotics, or medications, ESWT is sometimes a next-step option before considering surgery. It typically requires a series of sessions and may cause temporary discomfort, but many patients experience meaningful improvement over time.
9. Minimally invasive surgery (when needed)
While many people manage bone spur symptoms without an operation, there are times when surgery is the most practical route—especially if conservative treatment has failed over several months and your daily function is limited.
When surgery is considered
- Severe, persistent pain despite at least 3–6 months of non-surgical care
- Nerve compression causing weakness, numbness, or bowel/bladder issues (spine)
- Major limits in mobility or ability to work, walk, or sleep
Surgical options vary by location:
- Heel spur removal with release of tightened plantar fascia
- Shoulder decompression to remove spurs that are impinging the rotator cuff
- Spinal decompression to shave bone spurs pressing on nerves or the spinal cord
- Arthroscopic debridement in knees or ankles
Modern techniques are often minimally invasive, with small incisions and faster recovery times. Surgery doesn’t prevent new spurs from forming, so it’s still essential to address underlying mechanics and lifestyle factors.
Making your bone spur treatment plan work
Because every bone spur and every body is different, the best results usually come from combining several of these approaches rather than relying on just one.
Here’s a simple way to think about it:
-
Reduce inflammation and pain
- NSAIDs (oral or topical), ice, activity modification
- Possible corticosteroid injection if pain is severe
-
Correct mechanics and support the area
- Physical therapy, stretching, strengthening
- Orthotics, bracing, footwear changes
-
Support long-term joint health
- Weight management and low-impact exercise
- Good posture and body mechanics in daily activities
-
Escalate only if necessary
- Consider shockwave therapy or other advanced options
- Discuss surgery if conservative measures fail and quality of life is significantly impacted
Work closely with your healthcare provider, podiatrist, or physical therapist to tailor a plan to your specific bone spur location and overall health.
Frequently asked questions about bone spur treatment
1. Can a bone spur go away on its own?
A bone spur itself rarely “disappears” without surgical removal. However, the pain from a bone spur can improve significantly or even resolve with conservative care. By reducing inflammation, improving joint mechanics, and supporting the area properly, many people reach a point where they’re no longer bothered by the spur, even though it’s still present on imaging.
2. What is the best non-surgical treatment for a heel bone spur?
For a heel bone spur, the most effective non-surgical plan usually combines:
- Calf and plantar fascia stretching
- Supportive shoes and custom orthotics or heel cups
- Short-term NSAIDs or topical anti-inflammatories
- Night splints to reduce morning pain
- Activity modification (less high-impact, more low-impact exercise)
If these measures don’t help after several months, a podiatrist might suggest shockwave therapy or evaluate you for surgical options.
3. When should I worry about a bone spur in my spine?
Most spinal bone spurs are found incidentally on X-rays or MRIs and never cause symptoms. You should seek prompt medical attention if you have:
- Persistent back or neck pain combined with leg or arm weakness
- Numbness, tingling, or burning that radiates down a limb
- Problems with balance or walking
- Changes in bowel or bladder control
These can be signs that a bone spur is compressing nerves or the spinal cord, and you may need further evaluation and possibly more urgent treatment.
Take the next step toward bone spur relief
Living with a bone spur doesn’t have to mean living in constant pain or rushing into surgery. From targeted physical therapy and better footwear to shockwave therapy and, when needed, minimally invasive procedures, you have a full spectrum of proven options to reduce discomfort and regain your mobility.
If bone spur pain is limiting your work, hobbies, or sleep, talk with a healthcare professional about a personalized plan that starts with conservative care and escalates only if necessary. The sooner you address the mechanics, inflammation, and lifestyle factors involved, the sooner you can move with confidence and get back to the activities you enjoy.