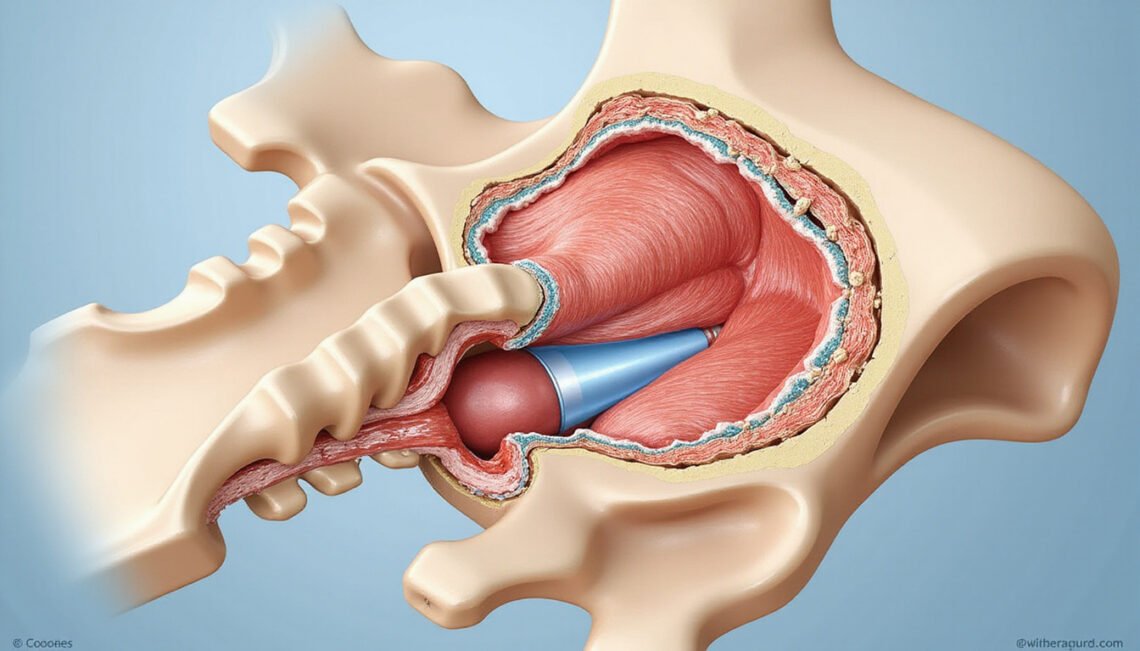
A caudal epidural is a targeted pain-relief procedure that delivers medication into the epidural space at the base of the spine, near the tailbone. It’s commonly used to treat lower back pain, sciatica, and leg pain that haven’t improved with rest, physical therapy, or medications. If you’re considering this injection or your doctor has recommended one, understanding how it works, what to expect, and the potential risks can help you decide with confidence.
What Is a Caudal Epidural?
A caudal epidural is a type of epidural steroid injection performed through the opening at the bottom of the spine called the sacral hiatus. Through this opening, a pain specialist can guide a needle into the epidural space and deliver:
- A corticosteroid (to reduce inflammation)
- A local anesthetic (to provide immediate numbing and pain relief)
- Sometimes a saline solution (to help flush inflammatory chemicals)
This approach allows medication to spread upward in the epidural space, targeting inflamed nerve roots that cause lower back and leg pain.
Conditions a Caudal Epidural Can Treat
Doctors often recommend a caudal epidural injection for pain that starts in the lower back and may radiate to the buttocks, thighs, or legs. Common conditions include:
- Lumbar disc herniation – when a disc bulges or ruptures, pressing on spinal nerves
- Lumbar spinal stenosis – narrowing of the spinal canal that compresses nerve roots
- Sciatica – pain, tingling, or numbness traveling along the sciatic nerve down the leg
- Degenerative disc disease – disc wear-and-tear causing chronic low back pain
- Post-surgical back pain – persistent pain after a prior back surgery
- Facet joint arthritis or inflammation – affecting the joints that connect vertebrae
A caudal epidural is typically considered after conservative treatments—such as physical therapy, anti-inflammatory medications, and activity modification—haven’t provided enough relief.
Who Is a Good Candidate for a Caudal Epidural?
You may be a candidate for a caudal epidural if:
- Your pain is significant enough to limit work, exercise, or daily activities.
- Imaging (MRI, CT, or X-ray) and clinical exam suggest nerve inflammation or compression in the lower spine.
- You’ve tried noninvasive treatments for several weeks with only partial or short-term improvement.
- You’re trying to avoid or delay back surgery.
On the other hand, you may not be a good candidate if you have:
- An active infection (especially near the injection site)
- Uncontrolled bleeding problems or are on certain blood thinners
- Uncontrolled diabetes or severe heart/lung disease (depending on your doctor’s assessment)
- Severe allergy to contrast dye, steroids, or local anesthetics previously used
Your pain management specialist or spine doctor will review your medical history and medications, and may order updated imaging to confirm that the pain source is likely to respond to a caudal epidural.
How Does a Caudal Epidural Work?
A caudal epidural relieves pain through three main mechanisms:
-
Reducing inflammation
Corticosteroids are powerful anti-inflammatory medications. When delivered directly around irritated spinal nerves, they can decrease swelling, chemical irritation, and nerve sensitivity. -
Interrupting pain signals
The local anesthetic temporarily numbs the involved nerve roots, which can reduce pain signals traveling to the brain and help break the cycle of pain–muscle spasm–more pain. -
Improving mobility and rehab participation
With better pain control, patients can move more freely, engage better in physical therapy, and strengthen core and back muscles—often leading to longer-term functional improvement.
The goal isn’t just to “mask” pain but to calm the underlying inflammation enough for your body to heal and for you to rebuild strength and mobility.
What to Expect Before, During, and After the Procedure
Before Your Caudal Epidural
Your healthcare team will provide specific instructions, which may include:
- Whether to hold blood thinners (e.g., warfarin, clopidogrel, some newer agents) several days in advance, under your prescribing doctor’s guidance.
- Whether you need to fast (no food or drinks) for a certain period if sedation will be used.
- Which medications you should continue taking (such as blood pressure or heart medications).
You’ll be asked to sign a consent form and may undergo a brief physical exam on the day of the injection.
During the Caudal Epidural Procedure
The actual procedure usually takes 10–20 minutes, with total visit time longer for preparation and recovery. It typically goes like this:
- You lie on your stomach on a procedure table.
- The lower back and sacral area (near the tailbone) are cleaned with antiseptic solution.
- The skin is numbed with a small injection of local anesthetic.
- Using fluoroscopy (live X-ray) guidance, the doctor inserts a needle through the sacral hiatus into the epidural space.
- Contrast dye is injected to confirm correct needle position and spread of medication.
- The steroid and local anesthetic solution is slowly injected.
- The needle is removed, the skin is cleaned, and a small bandage is placed.
Mild pressure or a brief “electric” sensation into the legs can occur but usually resolves quickly. If you experience severe pain at any point, tell your doctor immediately so they can adjust.
Immediately After the Injection
You’ll be monitored for 15–30 minutes. Common experiences include:
- Numbness or heaviness in the legs for a short time
- Reduced pain due to the local anesthetic
- Mild soreness at the injection site
Because of temporary weakness or numbness, most clinicians recommend that you do not drive yourself home. Arrange for a ride, especially if you received sedation.
How Long Does Pain Relief Last?
Pain relief after a caudal epidural varies widely:
- You may notice immediate relief from the local anesthetic that lasts a few hours.
- The steroid typically starts working within 24–72 hours, with peak benefit by about 1–2 weeks.
- Relief can last from several weeks to several months; in some cases, longer.
Some patients need a series of injections (often up to three, spaced several weeks apart) to achieve optimal improvement. Most guidelines recommend limiting the total number of epidural steroid injections per year to reduce steroid-related side effects—commonly no more than 3–4 per region annually (source: American Society of Interventional Pain Physicians, ASIPP).

Potential Benefits of a Caudal Epidural
Key benefits may include:
- Reduced lower back and leg pain
- Improved ability to walk, sit, and stand
- Less reliance on oral pain medications
- Better participation in physical therapy and exercise
- Possible delay or avoidance of surgical intervention
A caudal epidural is not a cure for structural spine problems, but it can be an important part of a comprehensive pain management plan.
Risks and Side Effects of Caudal Epidural Injections
Caudal epidurals are generally considered safe when performed by trained specialists, but no procedure is risk-free. Understanding the possible side effects helps you make an informed decision.
Common, Usually Mild Side Effects
These typically resolve within a few days:
- Soreness or bruising at the injection site
- Temporary increase in pain before improvement
- Headache or lightheadedness
- Flushing, facial warmth, or mood changes from steroids
- Trouble sleeping for a night or two after steroid injection
Less Common but More Serious Risks
These complications are rare, but important to know:
- Infection – at the skin, deeper tissues, or rarely, epidural abscess
- Bleeding or hematoma – more likely if on blood thinners or with clotting disorders
- Dural puncture (“wet tap”) – may cause a spinal headache
- Nerve injury – from direct trauma, pressure, or hematoma
- Allergic reaction – to contrast dye, anesthetic, or steroid
- Steroid-related systemic effects – temporary rise in blood sugar, fluid retention, mood swings, menstrual irregularities
Call your doctor or seek urgent care if you experience:
- New or worsening leg weakness, numbness, or trouble walking
- Loss of bladder or bowel control
- Fever, severe back pain, or redness/swelling at the injection site
- Severe, persistent headache that improves when lying down
Your pain specialist will weigh these risks against the potential benefits, taking into account your overall health and medical history.
Recovery and Aftercare: What You Should and Shouldn’t Do
Right After Your Caudal Epidural
In the first 24 hours:
- Rest and avoid strenuous activity.
- Keep the bandage on as directed; you can usually remove it later the same day.
- Avoid soaking in a bath, hot tub, or pool; showers are usually allowed.
- Use ice packs for 15–20 minutes at a time if the injection site is sore.
Activity and Work
Many people return to light activities or work the next day, depending on job demands and how they feel. Guidelines commonly include:
- Avoid heavy lifting, intense bending, or twisting for 24–48 hours.
- Gradually resume normal activity as pain allows.
- Follow your provider’s specific restrictions if you have a physically demanding job.
Medications
Your doctor may recommend:
- Continuing regular medications unless told otherwise
- Using over-the-counter pain relievers (like acetaminophen) if needed, as approved
- Monitoring blood sugar closely if you have diabetes, since steroids can cause temporary increases
Maximizing the Benefits of a Caudal Epidural
A caudal epidural works best when combined with a comprehensive treatment plan. To get the most from your injection:
-
Engage in physical therapy.
Once pain improves, focus on core strengthening, flexibility, and posture training. -
Maintain a healthy weight.
Extra body weight increases stress on the spine and can worsen symptoms. -
Stay active.
Low-impact exercise (walking, swimming, stationary cycling) helps keep muscles strong and joints mobile. -
Practice proper body mechanics.
Learn safe ways to lift, bend, and twist to protect your back. -
Manage underlying conditions.
Control diabetes, osteoporosis, and other chronic conditions that may affect the spine and healing.
Your provider may also discuss additional interventional options if pain persists, such as other types of epidural injections, facet joint injections, nerve blocks, radiofrequency ablation, or surgical consultation.
FAQ: Caudal Epidural Injections, Pain Relief, and Safety
1. How is a caudal epidural injection different from other epidural steroid injections?
All epidural steroid injections deliver medication into the epidural space, but caudal epidural injections enter through the tailbone area, while lumbar or transforaminal injections use different pathways in the lower back. The caudal route can be useful if prior surgeries or scar tissue make other approaches more difficult, or when broad coverage of multiple lumbar nerve roots is desired.
2. How often can I safely get caudal epidural steroid injections for back pain?
Most specialists limit caudal epidural steroid injections to a few per year—often no more than 3–4 per spinal region—depending on your response and your overall health. This limit helps reduce potential steroid-related side effects such as bone thinning, weight gain, and blood sugar changes. Your doctor will tailor the schedule to your needs and monitor for side effects.
3. Will a caudal epidural block cure my sciatica or herniated disc?
A caudal epidural block doesn’t “cure” the underlying structural problem, like a disc herniation or spinal stenosis. Instead, it aims to decrease inflammation and nerve irritation, providing pain relief and improved function. For some people, this relief, combined with physical therapy and lifestyle changes, is enough to manage the condition long-term. Others may still need additional procedures or surgery if significant nerve compression remains.
Take the Next Step Toward Pain Relief
Chronic lower back and leg pain can affect every part of your life—work, sleep, relationships, and mood. A caudal epidural may offer meaningful relief and help you regain mobility when other treatments haven’t been enough. If you’re struggling with persistent pain, don’t keep wondering whether this procedure might help. Schedule a conversation with a pain management specialist or spine doctor, review your imaging and symptoms together, and ask whether a caudal epidural injection fits your specific situation. With the right plan and expert guidance, you can move closer to lasting relief and a more active, comfortable life.