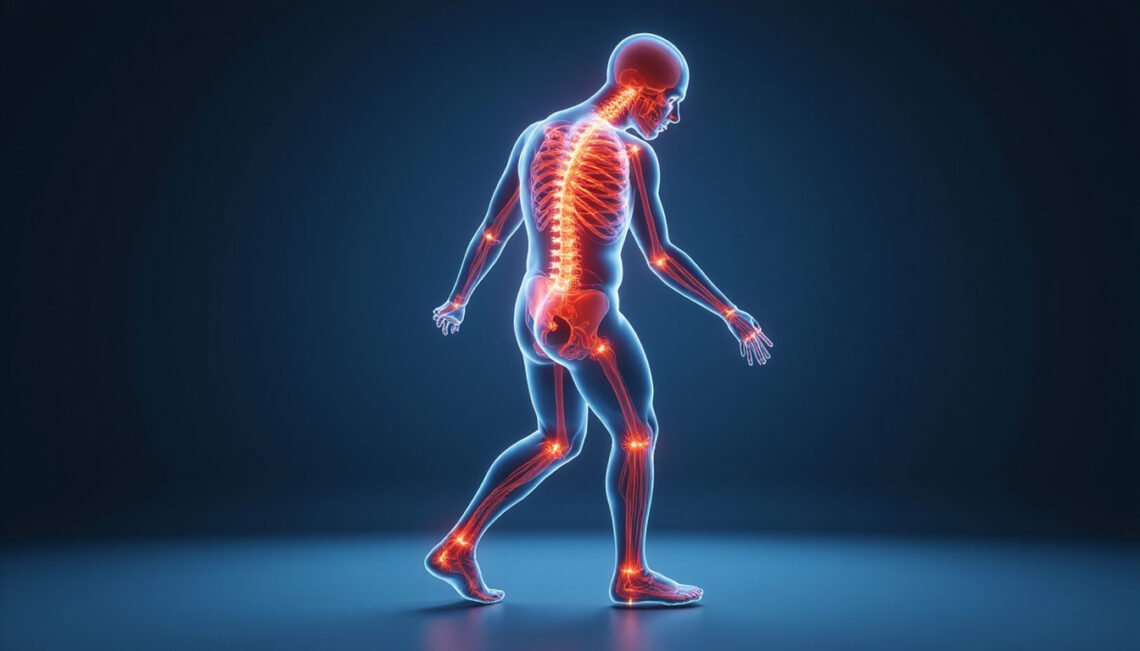
Leg weakness is a common but worrying symptom that can range from mild heaviness to sudden inability to stand. If you’re searching for answers about leg weakness, this guide explains eight hidden causes, what warning signs to watch for, and practical relief tips you can use today.
What does leg weakness mean?
Leg weakness describes reduced strength or control in one or both legs. It can feel like heaviness, numbness, clumsiness, or true loss of power when you try to walk, climb stairs, or stand up. Leg weakness can come on suddenly or develop gradually over weeks to months. Because it can signal anything from a temporary strain to a serious neurological or vascular condition, it’s important to take the symptom seriously and understand possible causes.
8 hidden causes of leg weakness
Below are eight less obvious — or often overlooked — causes of leg weakness. Each can affect strength and mobility in different ways.
- Nerve compression (radiculopathy)
- When a spinal disc bulges or degenerates, it can press on nerve roots that serve the legs, causing pain, tingling, and weakness in specific muscle groups.
- Peripheral neuropathy
- Damage to peripheral nerves from diabetes, toxins, or autoimmune disease can reduce muscle strength and coordination in the legs.
- Stroke or transient ischemic attack (TIA)
- A stroke can produce sudden, one-sided leg weakness often accompanied by facial droop or speech difficulties. TIAs cause similar but temporary symptoms and are a medical emergency.
- Multiple sclerosis (MS)
- MS causes immune attacks on the central nervous system, producing episodic leg weakness, spasticity, and balance problems.
- Spinal stenosis
- Narrowing of the spinal canal can compress the spinal cord or nerves, often causing leg weakness and pain that worsens when walking and improves with sitting.
- Myopathies and muscular dystrophies
- Primary muscle diseases can cause progressive leg weakness, usually without sensation changes, and may involve family history.
- Vascular problems (peripheral artery disease)
- Poor blood flow to the legs can cause cramping and fatigue with exertion and, in advanced cases, leg weakness or skin changes.
- Electrolyte imbalances and medications
- Low potassium, calcium, or magnesium, as well as certain drugs (statins, some blood pressure meds), can cause muscle weakness that affects the legs.
How doctors determine the cause
A clear history and focused exam point to the likely cause. Your clinician will ask about onset (sudden vs. gradual), pattern (one leg vs. both), associated symptoms (pain, numbness, vision or speech changes), medication use, and medical history (diabetes, autoimmune disease). Common diagnostic steps include:
- Neurological exam to test reflexes, strength, and coordination.
- Blood tests for glucose, electrolytes, and markers of inflammation.
- Imaging such as MRI of the spine or brain if nerve compression or stroke is suspected.
- Nerve conduction studies and electromyography (EMG) for peripheral neuropathy or myopathy.
- Vascular tests like ankle-brachial index (ABI) for suspected peripheral artery disease.
For trustworthy, in-depth information on muscle weakness evaluation, see the Mayo Clinic overview of muscle weakness (Mayo Clinic).
Warning signs that require immediate medical attention
Certain features with leg weakness should prompt an urgent medical visit or 911 call:
- Sudden, severe one-sided leg weakness, especially with facial droop, slurred speech, or confusion (possible stroke).
- Rapidly worsening weakness over hours to days.
- Loss of bladder or bowel control, or numbness in a saddle distribution (possible spinal cord compression).
- Fever with leg weakness (possible infection).
- Severe, unrelenting pain with weakness after trauma.
Simple relief tips you can try now
If your leg weakness is mild and not accompanied by red-flag signs, try these practical strategies to reduce symptoms and improve safety:
- Rest and paced activity
- Avoid strenuous exertion until you know the cause. Short, frequent walks can help circulation without overtaxing weak muscles.
- Optimize posture and ergonomics
- Use supportive footwear and avoid uneven terrain. When sitting, keep feet flat and avoid crossing legs for long periods.
- Home strengthening and mobility exercises
- Try gentle quadriceps and hamstring isometric contractions, ankle pumps, and seated marches. Progress gradually and stop if pain increases.
- Manage blood sugar and electrolytes
- People with diabetes should keep blood sugar within target ranges. If you suspect low potassium or other imbalances (weakness with cramps), see a clinician for testing.
- Medication review
- Bring a list of current medicines to your provider — some drugs can cause or worsen muscle weakness.
- Assistive devices for safety
- Canes or walkers reduce fall risk while you recover or await diagnosis.
Practical prevention and long-term care
Preventing recurrent episodes of leg weakness depends on the underlying cause, but these general measures help most people:
- Control chronic conditions (diabetes, hypertension, cholesterol) through diet, meds, and regular care.
- Stay active with a mix of strength, balance, and aerobic exercises; physical therapy can tailor a safe program.
- Avoid smoking, which worsens vascular disease.
- Maintain a healthy weight to reduce strain on muscles and spine.
- Have routine medication reviews with your provider.
When to see a specialist
Your primary care clinician may refer you to a neurologist, physiatrist (rehab doctor), vascular surgeon, or orthopedic/spine specialist depending on suspected cause. Early referral is important for progressive or unexplained weakness to prevent permanent impairment.

One bulleted list: quick signs to log before your appointment
- When did weakness start (date/time)?
- Which leg(s) and specific muscles feel weak?
- Any pain, numbness, or tingling? Where?
- Recent infections, new medications, or injuries?
- Changes in bladder or bowel control?
- Family history of neuromuscular disease?
Short FAQ
Q: Why does my leg feel weak but not painful?
A: Isolated leg weakness without pain can point to nerve or muscle conditions (like myopathy or neuropathy) or vascular insufficiency. A medical evaluation with neurological and muscle testing helps identify the cause.
Q: Can leg weakness be permanent?
A: Some causes of leg weakness — such as untreated nerve damage, advanced muscular dystrophy, or severe stroke — can produce lasting weakness. Early diagnosis and rehabilitation improve outcomes and may prevent permanent disability.
Q: What should I do for sudden leg weakness?
A: Sudden leg weakness could be a medical emergency. If it’s accompanied by facial droop, speech problems, confusion, or rapid deterioration, call emergency services immediately. Otherwise, seek urgent evaluation the same day.
Authority and evidence
This article summarizes common clinical causes and general management but is not a substitute for medical advice. For authoritative guidance on muscle weakness evaluation and causes, see the Mayo Clinic’s overview on muscle weakness (Mayo Clinic).
Conclusion and call to action
Leg weakness is a symptom with many faces — from temporary fatigue to signs of serious disease. If you’ve noticed unexplained or worsening leg weakness, don’t wait: log your symptoms, review your medications, and make an appointment with your primary care clinician. Early testing and targeted treatment can restore strength, reduce fall risk, and address underlying conditions before they worsen. If you’re experiencing sudden or severe weakness, seek emergency care right away. Take the first step today: schedule a professional evaluation and start a plan to regain strength and mobility.