If you or a loved one has been scheduled for myelography, it’s normal to feel unsure about what’s involved. Understanding the test, why it’s used, what happens before and after, and how to manage possible side effects can make the entire process less stressful and help you advocate for yourself.
This guide walks you through myelography in plain language—covering preparation, the procedure itself, risks, recovery tips, and common questions.
What Is Myelography?
Myelography (also called a myelogram) is a specialized imaging test that looks at your spinal cord, nerve roots, and the space around them (the spinal canal). It combines:
- A contrast dye (also called contrast medium) injected into the fluid around your spinal cord
- X-ray imaging, often followed by a CT scan
The contrast dye makes the spinal cord and nerves show up more clearly on images, helping doctors detect problems that may not be visible on standard X-rays or may need more detail than an MRI provides.
What Myelography Can Show
Myelography helps detect or evaluate:
- Herniated or bulging discs
- Spinal stenosis (narrowing of the spinal canal)
- Nerve root compression or irritation
- Spinal tumors or cysts
- Infections or inflammation involving the spinal cord
- Congenital (from birth) spinal abnormalities
- CSF (cerebrospinal fluid) leaks
It’s often used when MRI isn’t possible (for example, in people with certain pacemakers or metal implants), or when MRI and CT results don’t fully explain your symptoms.
Why Your Doctor Might Recommend a Myelogram
Your healthcare provider may suggest a myelogram if you have:
- Persistent back, neck, or leg pain that radiates down your arms or legs
- Numbness, tingling, or weakness in your limbs
- Difficulty walking, balance issues, or coordination problems
- Symptoms that don’t match previous imaging results
- A history of back or neck surgery, and new or worsening symptoms
Myelography can provide more precise information for:
- Deciding if surgery is needed
- Planning surgery (what level and what type)
- Evaluating previous spinal surgeries that didn’t relieve symptoms
- Guiding other treatments such as injections
How to Prepare for Myelography
Preparation is usually straightforward, but following instructions carefully helps keep you safe and improves image quality.
Medications and Medical History
Before the test, your medical team will review:
- Current medications (prescription, over-the-counter, supplements)
- Allergies, especially to iodine, contrast dye, or shellfish
- History of seizures, kidney disease, bleeding problems, or previous reactions to contrast
You may be asked to:
- Stop certain medications (especially some antidepressants, blood thinners, or diabetes drugs) temporarily
- Avoid aspirin or other blood thinners for a short time before the procedure, if safe
- Have blood tests to check kidney function or clotting, if needed
Always ask before stopping any prescription medication, particularly blood thinners or seizure medicine.
Eating and Drinking
Instructions may vary by facility, but commonly you will be told to:
- Avoid solid food for several hours before your myelogram
- Drink clear fluids up to a certain time (unless told otherwise)
- Stay well-hydrated the day before
Hydration helps your body handle the contrast dye and can lower the risk of post-procedure headaches.
Clothing and Personal Items
On the day of your myelography:
- Wear loose, comfortable clothing
- Leave jewelry and metal items at home if possible
- Bring a list of your medications and allergies
- Arrange for someone to drive you home; you shouldn’t drive yourself afterward
You’ll change into a hospital gown for the procedure.
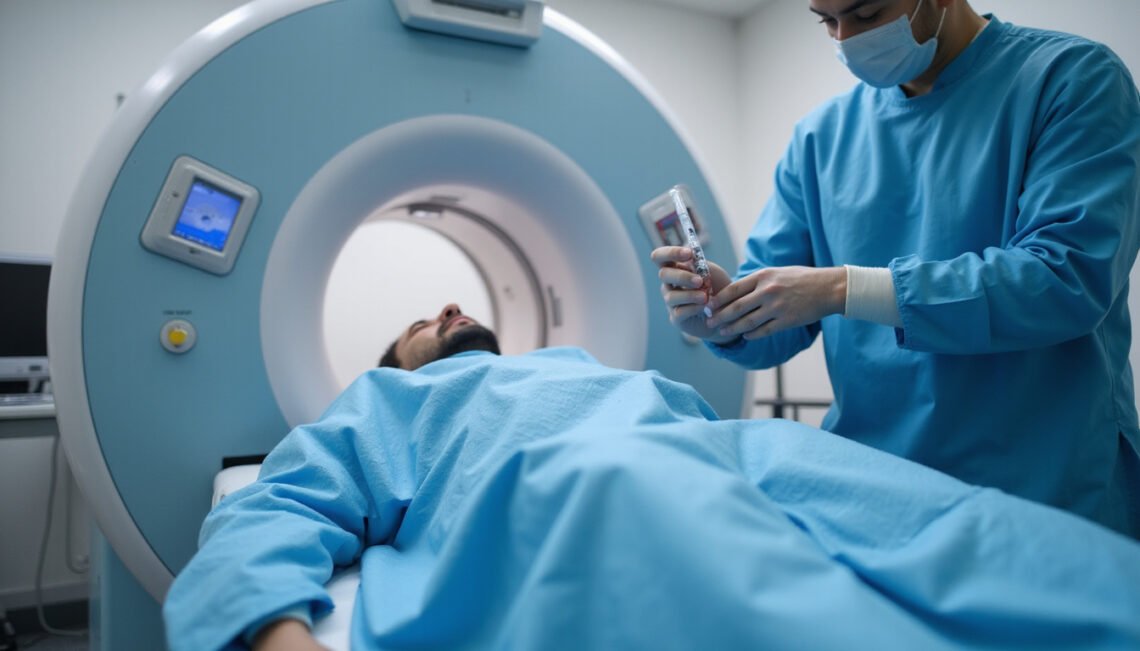
Step-by-Step: What Happens During a Myelogram
Knowing exactly what to expect can reduce anxiety. While details vary slightly by hospital, most myelography procedures follow a similar outline.
1. Check-In and Consent
You’ll check in, confirm your identity, and review your medical history. The radiologist or another doctor will:
- Explain the purpose of the test
- Review the risks and benefits
- Answer questions
- Ask you to sign a consent form
2. Positioning and Sterile Preparation
You’ll lie on an X-ray table, usually on your stomach or side, depending on which part of the spine is being studied (cervical/neck, thoracic/mid-back, or lumbar/lower back). The team will:
- Clean the skin on your lower back or neck with antiseptic
- Cover the area with sterile drapes
- Give local anesthetic (numbing medicine) to reduce needle discomfort
You’ll remain awake—sedation is not always necessary, but mild sedatives may be given if you’re very anxious.
3. Needle Placement and Contrast Injection
Using fluoroscopy (a live X-ray screen) for guidance, the radiologist will:
- Insert a thin needle into the spinal canal (the space containing cerebrospinal fluid). This is similar to a lumbar puncture (“spinal tap”).
- Confirm correct needle position, sometimes by letting a small amount of CSF drip out.
- Slowly inject the contrast dye into the CSF.
You might feel:
- Pressure or a brief ache in your back
- A warm or tingling feeling spreading down your legs or arms
Let the team know if anything feels very painful or unusual.
4. Moving the Contrast and Taking X-Ray Images
After the injection, the table may be tilted or you may be asked to gently roll from side to side. This helps the contrast travel up or down the spine to the area of interest. X-ray images are then taken in different positions.
This phase usually takes 15–30 minutes.
5. CT Scan (Often Immediately After)
Most modern myelography includes a CT myelogram:
- You’ll be moved to a CT scanner
- Additional images are captured, which provide highly detailed cross-sectional views of the spine and nerves
The CT portion usually lasts 10–20 minutes.
How Long Does Myelography Take?
In total, expect to be at the hospital or imaging center for 2–4 hours, including:
- Check-in and prep
- The myelogram and CT scan
- A post-procedure observation period
The injection and imaging themselves typically take under an hour.
Potential Risks and Side Effects of Myelography
Modern myelography is considered safe, but like any invasive test, it has potential risks. Understanding them helps you watch for warning signs afterward.
Common, Usually Mild Effects
These often resolve within a day or two:
- Headache, especially when sitting or standing
- Nausea or vomiting
- Dizziness or fatigue
- Mild back or neck soreness at the injection site
Post-myelogram headaches happen because the needle puncture can allow a small amount of CSF to leak, briefly reducing pressure in the brain and spinal canal.
Less Common but More Serious Risks
These are uncommon but important:
- Severe spinal headache that doesn’t improve with lying down, fluids, and pain medicine
- CSF leak that persists, sometimes requiring a procedure called an epidural blood patch to seal it
- Infection, such as meningitis, at the injection site or in the spinal fluid
- Allergic reaction to contrast dye (rash, itching, breathing difficulty)
- Bleeding in or around the spinal canal
- Nerve injury, which can cause new or worsening numbness, weakness, or severe pain
- Seizures, primarily in people with a history of seizures or those on certain interacting medications
According to major radiology guidelines, serious complications from myelography are rare when performed by experienced teams and when screening is done carefully (source: Radiological Society of North America).
When to Call Your Doctor or Seek Emergency Care
Contact your doctor or go to urgent care/ER if you experience:
- Severe headache that worsens when standing and doesn’t improve with rest
- Fever, stiff neck, or confusion
- Increasing back or neck pain, redness, or swelling at the injection site
- New numbness, weakness, or trouble walking
- Trouble urinating or loss of bowel/bladder control
- Shortness of breath, chest pain, or signs of a serious allergic reaction
Recovery After Myelography: Practical Tips
Most people go home the same day after a short observation period. Recovery is usually quick if you follow post-procedure instructions.

Immediately After the Procedure
You’ll likely be asked to:
- Lie flat or with your head slightly elevated for a few hours
- Drink fluids to help your body clear the contrast
- Avoid bending, heavy lifting, or straining
Nurses will monitor your blood pressure, pulse, and any early side effects.
At Home: Do’s and Don’ts
For the first 24–48 hours after myelography:
Do:
- Rest quietly; short, gentle walks are okay if you feel well
- Drink plenty of water or clear fluids
- Take pain relievers recommended by your doctor (usually acetaminophen)
- Keep the bandage clean and dry; follow instructions for showering
- Sleep with your head slightly elevated if you’re prone to headaches
Don’t:
- Perform heavy lifting, strenuous exercise, or vigorous bending/twisting
- Drive if you’re still dizzy or if you received sedatives
- Drink alcohol (it can worsen dehydration and headaches)
- Take medications your doctor told you to avoid until you’re cleared
Managing a Post-Myelogram Headache
If you develop a headache:
- Lie flat on your back, or slightly elevate your head if that feels better
- Hydrate well, including drinks with electrolytes or caffeine (if allowed)
- Use approved pain relievers
- Limit screen time and bright lights
If the headache is very severe or lasts more than 24–48 hours despite these measures, contact your doctor—it could be a sign of a significant CSF leak that might need an epidural blood patch.
How Results Are Interpreted and Shared
A radiologist—doctors specialized in imaging—will review your myelography images. They will:
- Look for compression of the spinal cord or nerves
- Evaluate the shape and width of the spinal canal
- Identify herniated discs, bone spurs, tumors, cysts, or signs of inflammation
- Compare with previous MRI or CT scans, if available
The radiologist sends a detailed report to the doctor who ordered the test (often a neurologist, neurosurgeon, spine surgeon, or pain specialist). You’ll usually:
- Receive results within a few days
- Discuss what they mean for your symptoms and treatment options at a follow-up appointment
Who Should Not Have Myelography?
Myelography may not be appropriate if you:
- Have a known severe allergy to iodinated contrast that cannot be managed with premedication
- Are pregnant (other imaging options are usually chosen to avoid radiation)
- Have active infection near the injection site
- Have uncontrolled bleeding disorders or are on blood thinners that cannot be safely paused
- Have certain conditions that raise seizure risk and are taking interacting medications
Your doctor will weigh the risks and benefits for your specific situation.
FAQs About Myelography and Myelograms
Is a myelogram painful?
Most people describe myelogram discomfort as similar to a blood draw in the back rather than severe pain. You’ll feel a pinch and pressure when the local anesthetic is injected and when the needle enters the spinal canal. During contrast injection you may feel warmth or tingling. Strong pain is not typical—tell the team immediately if you feel it.
How safe is CT myelography compared to MRI?
CT myelography is very effective for visualizing spinal canal problems, especially when MRI isn’t possible or doesn’t show enough detail. It does involve radiation and an invasive spinal injection, whereas MRI does not use radiation and isn’t invasive. However, for some patients—such as those with certain implants or complex post-surgical spines—CT myelography can provide clearer, more actionable information than MRI.
What should I avoid after a spinal myelography test?
After spinal myelography, avoid heavy lifting, intense exercise, and bending or twisting your spine for at least 24 hours (or as directed). Don’t drink alcohol, and don’t drive if you feel dizzy or were sedated. Focus on rest, hydration, and monitoring for symptoms like severe headache, fever, new weakness, or changes in bladder/bowel control, and report those to your doctor promptly.
Moving Forward After Myelography
Myelography is a precise tool that can clarify what’s happening inside your spine when symptoms are confusing or when other scans aren’t enough. By understanding the procedure, its risks, and how to recover well, you can approach it with more confidence and less anxiety.
If you’re scheduled for myelography or considering it:
- Write down your questions about the test, risks, and alternatives
- Review your medications with your doctor in advance
- Plan for a restful day or two afterward
- Ask how and when you’ll receive your results, and what the next steps might be
If you’re still unsure whether myelography is right for you, schedule a conversation with your healthcare provider or a spine specialist. An informed discussion about your symptoms, medical history, and imaging options is the best way to ensure you get the most appropriate, effective care for your spine and nerve health.