Transforaminal Epidural Injections: A Patient’s Guide to Quick Pain Relief
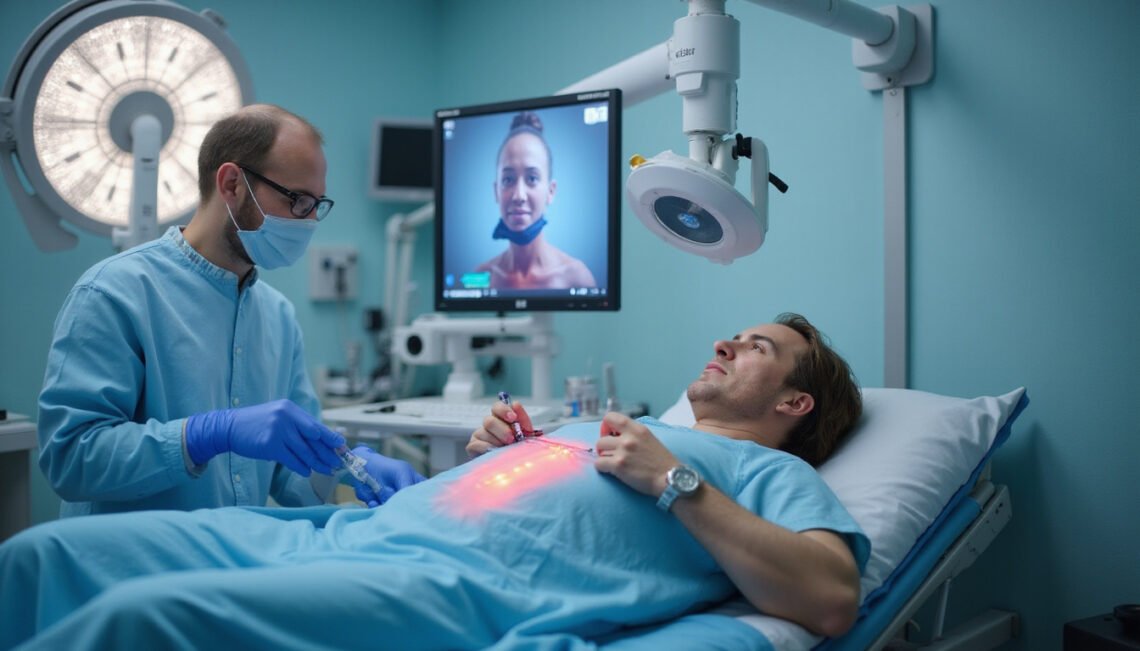
If you’re living with sharp, radiating back or leg pain from a pinched nerve, your doctor may recommend a transforaminal epidural injection. This minimally invasive procedure delivers targeted medication near irritated spinal nerves to reduce inflammation and pain—often much faster than oral medications alone. Understanding how it works, what to expect, and potential risks can help you feel more confident and prepared.
What Is a Transforaminal Epidural Injection?
A transforaminal epidural injection is a type of spinal injection in which medication (usually a steroid and a local anesthetic) is delivered into the epidural space through the opening where a spinal nerve exits the spine (the foramen).
- “Transforaminal”: through the foramen (the small opening where nerves leave the spinal canal)
- “Epidural”: the space surrounding the spinal cord and nerve roots
- Goal: reduce inflammation and swelling around a specific nerve root, thereby reducing pain, tingling, or weakness
Because the injection is guided to a specific nerve root, a transforaminal epidural can be more targeted than some other epidural techniques, which may spread medication more broadly.
Conditions That May Benefit from a Transforaminal Epidural
Your provider might recommend a transforaminal epidural injection if imaging and symptoms suggest nerve root irritation or compression. Common conditions include:
-
Lumbar or cervical disc herniation
A bulging or herniated disc can press on nearby nerve roots, causing sciatica-like symptoms, arm pain, or shooting pain into the buttocks or legs. -
Spinal stenosis
Narrowing of the spinal canal or nerve root openings can compress nerves, leading to pain, numbness, weakness, and burning sensations. -
Degenerative disc disease
Age-related disc changes can irritate adjacent nerves and cause chronic low back and leg pain. -
Facet joint cysts or arthritic changes
Bone spurs or cysts near the joints of the spine can crowd the nerve root exit, resulting in radiating pain. -
Failed back surgery syndrome
Persistent nerve pain after spine surgery may sometimes be relieved by a well-placed transforaminal epidural.
This procedure is usually considered when conservative treatments—such as physical therapy, oral anti-inflammatory medications, activity modification, and sometimes chiropractic care—haven’t provided sufficient relief.
How Does a Transforaminal Epidural Work?
The main therapeutic component of a transforaminal epidural is usually a corticosteroid, a powerful anti-inflammatory drug. It is often combined with a local anesthetic, which can provide short-term numbing relief and also helps confirm that the pain source has been accurately targeted.
Here’s how it helps:
-
Reduces inflammation
Steroids calm the inflammatory response around the irritated nerve root, which can decrease pain, swelling, and nerve sensitivity. -
Improves nerve function
Reducing pressure and inflammation can allow the nerve to transmit signals more normally, potentially reducing numbness or weakness. -
Breaks the pain cycle
Lowering pain can make it easier to move, stretch, and participate in physical therapy, which can further support long-term recovery. -
Diagnostic benefit
If your pain improves significantly after a transforaminal epidural, it confirms that the targeted nerve is indeed responsible for your symptoms.
Relief may begin within hours to days (due to the anesthetic) and often improves more fully over 3–7 days as the steroid effect builds.
Transforaminal Epidural vs. Other Epidural Injections
Several types of epidural steroid injections exist. A transforaminal epidural differs in approach and precision:
-
Interlaminar epidural
Medication is injected into the central epidural space between two vertebrae. The medicine spreads more diffusely and may reach multiple levels and both sides, but it is less targeted to a single nerve root. -
Caudal epidural
Medication is injected through a small opening near the tailbone into the epidural space. This can be helpful when scarring or anatomy makes other approaches difficult. -
Transforaminal epidural
Medication is guided to the specific foramen of the affected nerve root, usually on one side. This often allows for more precise pain targeting, especially in radicular pain (sciatica, arm pain) (source: Spine-health).
Your provider will recommend the most appropriate type based on your anatomy, imaging results, symptoms, and previous treatment response.
Preparing for a Transforaminal Epidural Injection
Before the procedure, your healthcare team will review your medical history and medications. Common preparation steps include:
-
Medication review
You may be asked to pause blood thinners (e.g., warfarin, certain antiplatelet medications) for a defined period, with guidance from your prescribing doctor. -
Allergy check
Inform your provider about any allergies to contrast dye, local anesthetics, or steroids. -
Health conditions
Conditions such as diabetes, bleeding disorders, or active infections can affect timing and safety of a transforaminal epidural. -
Eating and drinking
Some centers allow a light meal, while others prefer you to fast for several hours—follow the instructions given to you. -
Transportation
Arrange for someone to drive you home, especially if you’ll receive sedative medication.
Bring a list of current medications and questions you want to ask. Being informed can reduce anxiety and help you participate in shared decision-making.
What Happens During the Procedure?
A transforaminal epidural injection is typically an outpatient procedure and may take 15–30 minutes, plus recovery time. Here’s the usual sequence:
-
Positioning
You’ll lie face down (for lumbar) or on your back/side (for cervical) on a procedure table. -
Skin cleaning and local anesthesia
The injection site is cleaned with an antiseptic. The doctor injects a small amount of local anesthetic to numb the skin and deeper tissues; this may sting briefly. -
Imaging guidance
Using fluoroscopy (live X-ray) or sometimes CT guidance, the physician guides a thin needle toward the appropriate foramen, near the affected nerve root. -
Contrast dye
A small amount of contrast dye may be injected to confirm correct needle placement and ensure medication will flow into the desired area. -
Medication injection
The steroid and local anesthetic mixture is slowly injected. You might feel slight pressure or temporary reproduction of your usual pain—this can actually confirm that the right nerve is being treated. -
Post-procedure monitoring
You’ll rest in a recovery area for 15–30 minutes while staff monitor your blood pressure and symptoms. Most patients go home the same day.
Sedation (light calming medication through an IV) is sometimes used but not always necessary. Many patients manage well with just local anesthetic.
What to Expect After a Transforaminal Epidural
Recovery is usually quick. Typical experiences include:
-
Numbness or weakness
Temporary numbness or heaviness in the limb supplied by the injected nerve can occur due to the local anesthetic. This usually resolves within a few hours. -
Soreness at the injection site
Mild soreness or bruising is common and often improves within 1–2 days. -
Pain relief timeline
- Immediate: Possible short-term relief from the local anesthetic (can last several hours).
- 1–3 days: Pain may return or fluctuate as the anesthetic wears off and the steroid is just beginning to work.
- 3–7 days: Many patients notice more significant, stable pain reduction as the steroid takes full effect.
-
Activity level
Most providers recommend light activity the day of the procedure, avoiding strenuous exercise or heavy lifting for 24 hours. You can typically resume normal activities the next day as tolerated.
Contact your provider promptly if you experience severe headache, fever, increasing redness or drainage at the injection site, new weakness, or loss of bladder/bowel control.
Potential Benefits and How Long Relief Lasts
A transforaminal epidural does not “fix” structural spinal problems, but it can provide important symptom relief and a window for healing.
Potential benefits include:
- Reduced radiating leg or arm pain
- Less reliance on oral pain medications
- Improved ability to walk, sit, sleep, or participate in daily activities
- Better tolerance for physical therapy and exercise
- Possible delay or avoidance of surgery for some patients
Duration of relief varies:
- Some patients experience relief for weeks.
- Many have benefit lasting several months.
- In some, pain relief may be limited or short-lived.
If successful, a transforaminal epidural can sometimes be repeated (commonly up to 3–4 times per year, depending on your overall health and provider’s protocol).
Risks and Side Effects of a Transforaminal Epidural
Although generally safe when performed by an experienced clinician, a transforaminal epidural injection—like any medical procedure—has potential risks.
Common, usually mild:
- Temporary increase in pain
- Injection site discomfort
- Mild headaches
- Flushing or facial warmth
- Sleep disturbance or mood changes from steroids
Less common but more serious:
- Infection (epidural abscess, meningitis)
- Bleeding or hematoma in the epidural space
- Nerve injury or increased nerve pain
- Allergic reaction to contrast dye or medications
- Very rare but serious neurologic complications, especially in high-risk areas like the cervical spine
Diabetic patients may notice temporarily higher blood sugar levels for several days due to steroids.
Discuss your specific risk profile with your provider. Ask how they minimize risks—for example, using real-time imaging, avoiding certain steroid types in high-risk areas, and following strict sterile technique.
When Is a Transforaminal Epidural Not Recommended?
A transforaminal epidural injection may not be suitable if you have:
- Uncontrolled bleeding disorders or are on certain blood thinners that can’t be safely paused
- An active infection (systemic or at/near the injection site)
- Severe, uncontrolled diabetes or heart disease (relative contraindications)
- Allergy to contrast dye, steroids, or local anesthetics (unless an alternative plan is developed)
- Signs of spinal cord compression or cauda equina syndrome requiring emergency surgery
In these cases, your medical team will help identify alternative treatments.
How to Make the Most of Your Pain Relief
A transforaminal epidural can offer a critical window of reduced pain. To maximize benefits:
-
Follow a structured physical therapy plan
Use improved comfort to strengthen core and back muscles, improve flexibility, and correct posture. -
Stay active within your limits
Gentle walking, stretching, and low-impact exercise often support spinal health and reduce stiffness. -
Address lifestyle factors
Weight management, smoking cessation, and ergonomic adjustments at work/home can reduce ongoing stress on your spine. -
Track your symptoms
Keep a simple pain and activity diary for a few weeks after the injection—this helps your provider evaluate effectiveness and plan next steps.
Frequently Asked Questions About Transforaminal Epidural Injections
1. How painful is a transforaminal epidural steroid injection?
Most people describe only mild to moderate discomfort. You’ll feel a brief sting from the numbing shot and some pressure as the transforaminal epidural needle is advanced. Short-lived reproduction of your usual leg or arm pain can occur when the nerve is reached. If you’re anxious, ask about light sedation options.
2. How long does a transforaminal epidural nerve root block last?
A transforaminal epidural nerve root block can provide relief ranging from a few weeks to several months. The local anesthetic wears off within hours, but the steroid can continue reducing inflammation for weeks. Results vary based on your specific condition, degree of nerve compression, and overall health.
3. Is a transforaminal epidural injection safe for chronic back and leg pain?
For many patients with nerve-related chronic back and leg pain, a transforaminal epidural injection is considered a safe and appropriate option when done by an experienced specialist. While risks exist, they are relatively low and are weighed against the potential benefits of improved function, reduced medication use, and possible avoidance of surgery.
Take the Next Step Toward Relief
Living with radiating back, leg, or arm pain can affect every aspect of your life—from work and sleep to relationships and mood. A well-planned transforaminal epidural injection may provide the quick, targeted relief you need to break the pain cycle and return to the activities you value. If your current treatments aren’t giving you the results you hoped for, talk with your spine specialist or pain management physician about whether this procedure fits your diagnosis, health status, and goals. With the right information and team, you can move closer to lasting comfort and better function.