Lower back pain that just won’t go away often gets blamed on “a bad back” or “a slipped disc.” But for a surprising number of people, the true culprit is SI joint dysfunction—a problem in the sacroiliac joints where your spine meets your pelvis. When this small but powerful joint is irritated or unstable, it can cause deep, aching pain in the low back, hips, and even down the leg. The good news: with the right diagnosis and a targeted plan, most people can dramatically reduce or even eliminate SI joint–related pain.
Understanding SI Joint Dysfunction
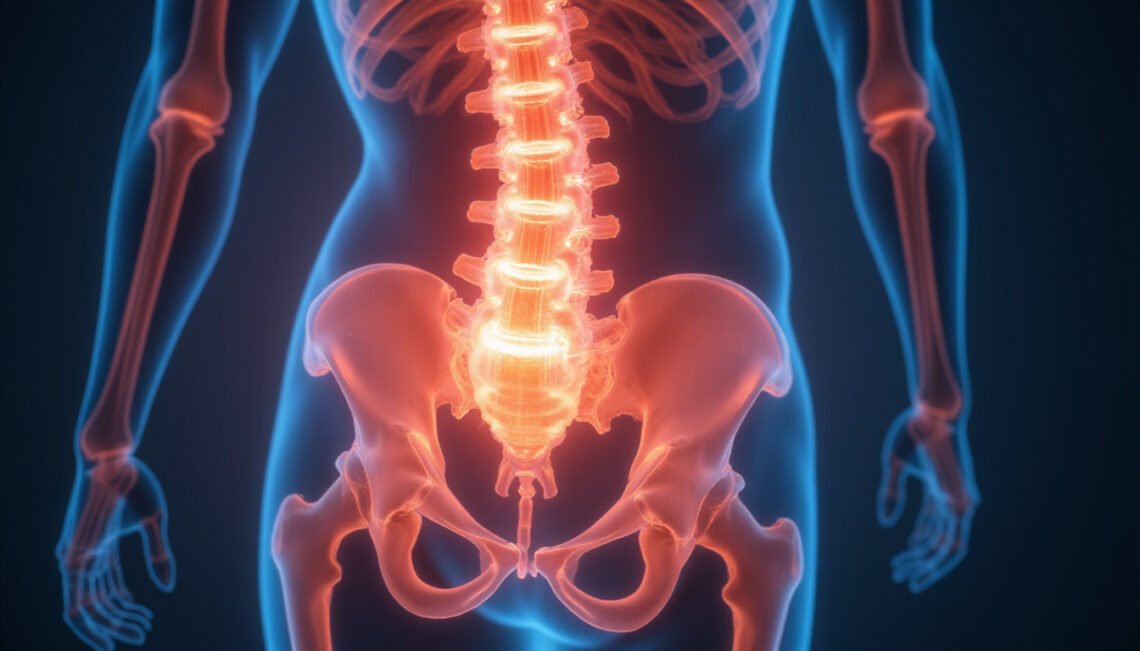
Your sacroiliac (SI) joints sit at the base of your spine, connecting the sacrum (tailbone) to the iliac bones of your pelvis. You have one on each side. They’re designed to be very stable, allowing only a few degrees of motion, but they play a huge role in bearing and transferring load between your upper body and legs.
SI joint dysfunction occurs when these joints move too much (hypermobility/instability) or too little (hypomobility/stiffness), or when the surrounding tissues become inflamed. This can come from:
- Trauma, such as a fall or car accident
- Pregnancy and childbirth
- Repetitive stress from sports or heavy lifting
- Leg length differences or scoliosis
- Spinal fusion surgery that increases load on the SI joints
Over time, the joint surfaces and surrounding ligaments can become irritated, leading to chronic pain.
Common Symptoms and How They Differ from Other Back Problems
SI joint pain is often misdiagnosed as a lumbar disc problem or “sciatica.” Recognizing the unique pattern of symptoms can help you and your provider narrow it down.
Typical signs of SI joint dysfunction include:
- Aching pain on one side of the low back or buttock (sometimes both, but often one-sided)
- Pain that may radiate into the groin, hip, or back of the thigh
- Pain worse when standing up from sitting, climbing stairs, or rolling over in bed
- Discomfort with prolonged standing or walking, often relieved somewhat by sitting
- Pain when putting weight on one leg (like standing on one leg to put on pants)
Red flags like numbness, significant weakness, or loss of bowel/bladder control point more toward spinal nerve compression and need urgent evaluation. SI joint dysfunction typically causes deep, aching pain, not sharp, shooting nerve pain all the way to the foot.
How SI Joint Dysfunction Is Diagnosed
There’s no single perfect test, so diagnosis usually relies on a combination of:
- Detailed history: What activities trigger your pain? Where exactly do you feel it?
- Physical exam: Your clinician may perform a series of “provocation tests” (like FABER, Gaenslen, thigh thrust) that stress the SI joint to see if your familiar pain is reproduced.
- Imaging: X-rays, CT, or MRI can help rule out other causes (fracture, disc herniation, hip arthritis), but they don’t always show SI problems clearly.
- Diagnostic injection: In some cases, a guided injection of local anesthetic into the SI joint is used. If your pain temporarily improves significantly, it supports the diagnosis (source: North American Spine Society).
Because many structures in the low back and pelvis can hurt in similar ways, it’s important to work with a provider experienced in spine and pelvic conditions—such as a physiatrist, orthopedic spine specialist, or well-trained physical therapist.
Proven Non-Surgical Strategies That Actually Work
Most people with SI joint dysfunction improve with conservative (non-surgical) care. The key is a comprehensive approach that addresses pain, mobility, stability, and daily habits.
1. Activity Modification and Body Mechanics
Your first step is to dial down the overload on your SI joint so it can calm down.
Helpful changes include:
- Avoiding heavy lifting or twisting through the low back
- Keeping loads close to your body and using your legs to lift
- Sitting with feet supported and hips slightly higher than knees
- Breaking up long periods of sitting or standing with movement breaks
- Getting in/out of the car or bed by moving your whole body as one unit (log-rolling), instead of twisting
Temporary lifestyle adjustments can make a big difference in reducing daily irritation while you build strength and stability.
2. Targeted Physical Therapy
Evidence strongly supports physical therapy as a first-line treatment for SI joint dysfunction. A skilled PT will usually combine manual techniques with a structured exercise program, phased in carefully.
Common PT components:
- Manual therapy: Gentle mobilizations, soft tissue work, and sometimes manipulation to improve joint alignment and reduce muscle tension
- Stabilization training: Focus on the deep core (transverse abdominis), pelvic floor, and gluteal muscles to support the SI joint
- Stretching: Especially hip flexors, hamstrings, piriformis, and lower back, if they’re tight and pulling the pelvis out of balance
- Gait and posture training: Correcting asymmetries in how you stand, walk, and move through daily tasks
Consistency matters more than intensity. For chronic SI joint dysfunction, expect at least 6–12 weeks of regular PT and home exercises to see reliable improvement.
3. Medications and Topical Options
Medication doesn’t fix the underlying problem, but it can help manage symptoms while you work on the root causes.
Common options include:
- NSAIDs (ibuprofen, naproxen) to reduce pain and inflammation, if you can take them safely
- Acetaminophen for pain relief when NSAIDs are not appropriate
- Topicals such as diclofenac gel or lidocaine patches for targeted relief over the painful area
Always discuss long-term use and possible side effects with your healthcare provider, especially if you have kidney, liver, heart, or GI concerns.
4. SI Joint Belts and Braces
For some people—especially those with hypermobility or postpartum instability—an SI joint belt worn low around the pelvis can:
- Provide external compression and stability
- Reduce pain during walking or standing
- Support the area while you strengthen the surrounding muscles
Belts are usually a short-term assist, not a permanent solution. Your PT can help you choose the right type and fit.

Exercise Strategies: Strength Without Strain
If you have SI joint dysfunction, the goal of exercise is to stabilize, not aggravate. That means starting small and focusing on quality of movement.
Gentle Stabilization Exercises
With clearance from your provider or PT, the following categories are often helpful:
- Deep core activation:
- Abdominal bracing in supine (lying on your back)
- Dead bug variations with small, controlled movements
- Glute strengthening:
- Glute bridges
- Clamshells with or without a resistance band
- Side-lying leg raises
- Hip mobility and balance:
- Hip flexor and piriformis stretches
- Standing hip abduction/adduction
- Single-leg balance progressing to dynamic movements
Activities to Use Caution With
Until your SI joint is more stable, many people need to modify or avoid:
- High-impact exercises (running, jumping, plyometrics)
- Heavy barbell squats and deadlifts
- Deep twisting motions (certain yoga poses, golf swings)
- Asymmetrical loading (carrying heavy bags on one side)
Work with your PT to safely reintroduce higher-level activities and sports as your symptoms improve.
Interventional Treatments: When Conservative Care Isn’t Enough
If several months of structured conservative treatment don’t provide adequate relief, interventional options may be considered.
1. Image-Guided Injections
Two main types are used:
- Corticosteroid injections into the SI joint can significantly reduce inflammation and pain for weeks to months. This may enable you to participate more fully in rehab.
- Radiofrequency ablation (RFA) targets the small nerves that carry pain signals from the SI joint. By “deactivating” them with heat, RFA can offer pain relief for 6–12 months or more in some cases.
These procedures are typically done under X-ray or ultrasound guidance by a pain management specialist or interventional physiatrist.
2. SI Joint Fusion Surgery
Surgery is reserved for carefully selected patients with:
- Clear, confirmed SI joint dysfunction as the primary pain source
- Persistent, disabling pain despite extensive conservative treatment
- Strong but temporary relief from diagnostic SI joint injections
Modern SI joint fusion is minimally invasive, using small implants to stabilize the joint. While many people experience significant pain reduction, it’s still major surgery with risks and a recovery period, so it should be considered only after thorough discussion and second opinions when possible.
Prevention and Long-Term Management
Even after pain is under control, SI joint dysfunction can flare if old habits return. Long-term success hinges on maintenance and prevention:
- Continue a core and hip strengthening routine 2–3 times a week
- Maintain healthy body weight to reduce load on the joints
- Use proper body mechanics with lifting and bending
- Vary your posture—avoid long periods in one position
- Address contributing factors like leg length differences with shoe inserts if recommended
- Manage related conditions, such as inflammatory arthritis, with your rheumatologist
Think of your SI joint as a key link in your kinetic chain: when the muscles around it stay strong and coordinated, the joint is far less likely to become symptomatic again.
FAQ: SI Joint–Related Questions
1. What is sacroiliac joint dysfunction and how is it different from a herniated disc?
Sacroiliac joint dysfunction refers to abnormal motion or inflammation of the sacroiliac joints at the base of your spine. It usually causes deep, aching pain in the low back, buttocks, and sometimes the groin or upper thigh. A herniated disc, on the other hand, involves the discs between your vertebrae and often causes sharp, radiating nerve pain, numbness, or weakness down the leg. A careful exam and, in some cases, diagnostic injections help distinguish the two.
2. Can SI joint pain go away on its own?
Mild sacroiliac joint pain sometimes improves with rest and simple home measures, especially if caused by a short-term strain. However, chronic SI joint dysfunction often persists or recurs without targeted treatment to restore stability and proper mechanics. Early evaluation and a structured rehab plan greatly increase the chances of long-lasting relief.
3. What are the best exercises for sacroiliac joint pain relief?
The best exercises for sacroiliac joint pain typically focus on gentle core and hip strengthening, such as abdominal bracing, glute bridges, clamshells, and targeted stretches for the hip flexors and piriformis. The ideal program is individualized based on your alignment, strength, and movement patterns, so working with a physical therapist is strongly recommended.
Take the Next Step Toward Ending Your SI Joint Pain
Living with daily low back and pelvic pain can drain your energy, limit your activities, and chip away at your quality of life. If your symptoms match those of SI joint dysfunction, you don’t have to accept them as “just getting older.” With an accurate diagnosis and a personalized plan—combining activity changes, focused physical therapy, and, when needed, interventional options—many people reclaim pain-free movement and confidence in their bodies.
Don’t wait for the pain to become your “new normal.” Reach out to a spine or pain specialist or a skilled physical therapist who understands SI joint conditions, and start a targeted program today. The sooner you address SI joint dysfunction at its source, the faster you can get back to walking, working, exercising, and living without chronic lower back pain calling the shots.