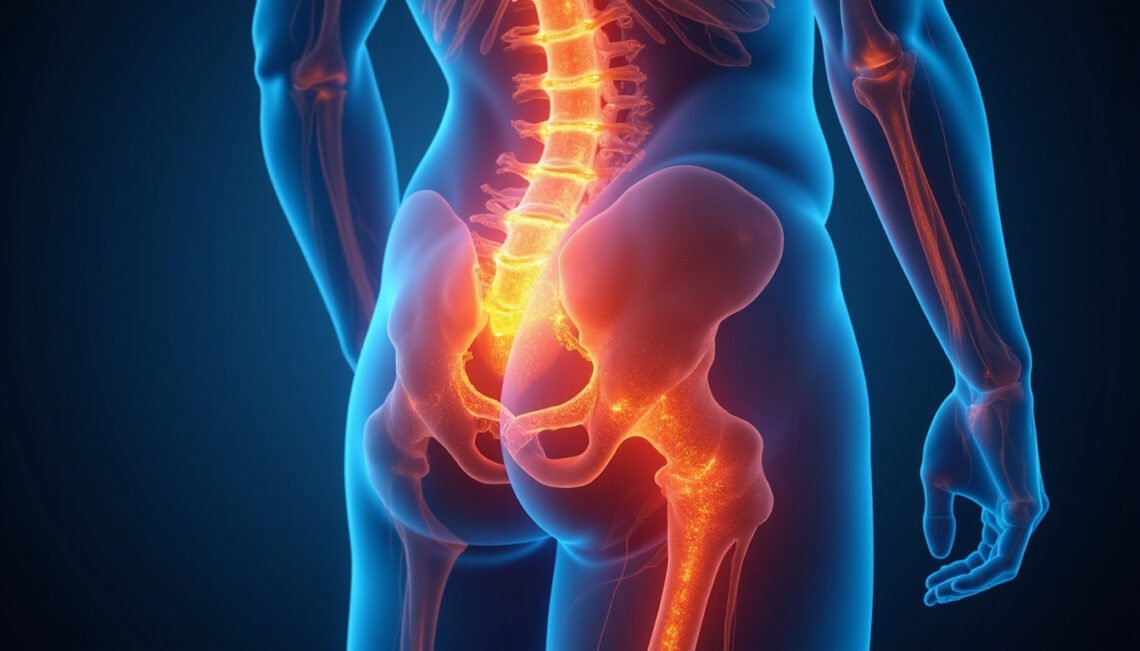
Cluneal nerve pain is an under‑recognized cause of stubborn low back and buttock pain that often gets misdiagnosed as a disc problem, SI joint issue, or simple muscle strain. Because the cluneal nerve is small and often overlooked on imaging, people can spend months or years chasing the wrong treatments. Understanding how this nerve works, why it becomes irritated, and what actually helps can be the key to finally getting relief.
What is the cluneal nerve?
The cluneal nerve is a group of sensory nerves that supply feeling to the skin over the lower back, buttocks, and upper portion of the hips. There are three main groups:
- Superior cluneal nerves – come from the upper lumbar spine (L1–L3) and wrap around to the upper buttocks.
- Middle cluneal nerves – arise from the sacral nerves (S1–S3) and supply the central buttock area.
- Inferior cluneal nerves – branch from the posterior femoral cutaneous nerve and supply the lower buttocks near the fold.
These nerves don’t move muscles; they transmit sensation, including pain, temperature, and touch, from the skin and connective tissues in the lower back and buttock area.
When one or more branches become compressed, stretched, or inflamed, the result is called cluneal nerve entrapment or cluneal neuralgia—a specific type of nerve pain that is often mistaken for other back problems.
Why cluneal nerve pain is often missed
Cluneal nerve issues can be tricky to pinpoint because:
- Standard X-rays and MRIs usually look normal.
- Symptoms overlap with sciatica, sacroiliac (SI) joint pain, or lumbar facet joint pain.
- Many practitioners are less familiar with cluneal neuralgia than with disc herniations or spinal stenosis.
As a result, people might go through repeated rounds of physical therapy, chiropractic care, or even spinal injections for “disc pain” without much improvement—because the true source is a small, irritated cluneal nerve near the back of the pelvis, not the spine itself.
Surprising causes of cluneal nerve pain
The cluneal nerve can be irritated by many everyday activities and medical conditions. Some of the most common and surprising triggers include:
1. Tight fascial bands and bony grooves
The superior cluneal nerve runs over the rim of the pelvis (iliac crest) and can get pinched as it passes through tight fibrous tunnels or fascial bands. Repetitive bending, twisting, or extended walking can cause irritation where the nerve crosses bone.
2. Prolonged sitting or “wallet neuropathy”
Sitting for long periods—especially on hard surfaces—can compress the middle and inferior cluneal nerves. Keeping a thick wallet in a back pocket can worsen pressure on these nerves, leading to one-sided buttock pain sometimes called “wallet sciatica,” even when the sciatic nerve is not the main issue.
3. Repetitive sports and training
Activities that involve frequent bending, torsion, or impact around the pelvis—such as running, rowing, cycling, weightlifting, or gymnastics—can strain the tissues that surround the cluneal nerve. Over time, small irritations add up to chronic nerve sensitivity.
4. Falls, minor trauma, and car accidents
Even if imaging doesn’t show a fracture or major injury, a fall onto the buttocks, a side impact, or seat belt traction in a car crash can stretch or bruise the cluneal nerve along the rim of the pelvis or sacrum.
5. Surgical scars and prior procedures
Back or pelvic surgeries, including:
- Lumbar spine surgery
- Hip surgery
- Sacroiliac joint fusion
- Bone graft harvest from the iliac crest
can create scar tissue that traps the cluneal nerve. In some people, this becomes a delayed source of chronic pain months or years after an otherwise successful procedure.
6. Posture, alignment, and muscle imbalance
Weak core and gluteal muscles, pelvic tilt, or leg-length differences can change how forces travel across the pelvis. Over time, this can cause micro-irritation of the cluneal nerves as they travel through surrounding ligaments and fascial tissue.
Key symptoms of cluneal nerve entrapment
Symptoms of cluneal nerve pain tend to follow a recognizable pattern, though it can vary by person and which branch is involved.
Common features include:
- Focal pain over the upper buttock or along the iliac crest (top of the pelvic bone), usually on one side but sometimes both.
- Pain that radiates sideways or slightly down into the buttock, but rarely below the mid-thigh.
- Sharp, burning, stabbing, or electric pain, often with tenderness to touch in a very specific spot.
- Worsening with certain positions, especially:
- Prolonged sitting
- Leaning backward
- Walking or standing for long periods
- Relief with rest, lying down, or changing positions.
People sometimes describe an area of:
- Numbness
- Tingling
- Hypersensitivity or “sunburned skin” feeling
over the lower back or upper buttock. This is consistent with the sensory distribution of the cluneal nerve.
How it differs from sciatica or disc pain
Cluneal nerve pain:
- Usually does not cause pain below the knee.
- Rarely causes true muscle weakness.
- Is often very localized to the upper buttock or iliac crest region.
- May have a clear “trigger point”—a small area that, when pressed, reproduces familiar pain.
Sciatica from a lumbar disc, by contrast, typically:
- Radiates down the back of the leg, often below the knee.
- May cause numbness, tingling, or weakness in a dermatomal pattern.
- Is more strongly provoked by coughing, sneezing, or spinal flexion.
How is cluneal nerve pain diagnosed?
There is no single definitive test, but a thorough evaluation usually includes:
-
Detailed history
- Location and character of pain
- Activities that worsen or relieve symptoms
- Prior injuries or surgeries to the back, pelvis, or hips
-
Focused physical exam
A clinician may:- Palpate (press) along the iliac crest and sacrum to find a small, very tender spot.
- Recreate pain by pressing where the superior cluneal nerve crosses the pelvic rim (often 7–8 cm from the spine).
- Perform a Tinel’s sign—tapping over the suspected nerve to trigger tingling or shooting pain.
-
Rule out other causes
- Basic imaging (X‑ray, MRI) to exclude fractures, major disc herniation, or severe hip/SI joint disease.
- Neurologic exam to check for muscle weakness or reflex changes.
-
Diagnostic nerve block
The most definitive step is often a cluneal nerve block:- A small amount of local anesthetic (sometimes with steroid) is injected near the suspected nerve.
- If pain relief is significant but temporary, it supports the diagnosis of cluneal nerve entrapment.
Clinical studies suggest superior cluneal nerve entrapment may be an underdiagnosed cause of low back pain in a notable subset of patients (source: National Library of Medicine).
Fast relief options: what really helps
For many people, cluneal nerve pain responds well to a combination of targeted treatments. The right plan depends on severity, duration, and underlying causes.

1. Activity modifications and posture changes
You can often reduce irritation quickly by changing daily habits:
- Avoid sitting on hard surfaces for long periods.
- Use a cushioned seat or donut pillow, especially if your pain worsens with sitting.
- Remove thick items (like a wallet or phone) from your back pockets.
- Alternate between sitting, standing, and short walks throughout the day.
These steps reduce direct pressure on the cluneal nerve, giving it a chance to calm down.
2. Targeted physical therapy
Work with a therapist familiar with pelvic and lumbar pain. A program may include:
- Gentle stretching of the lower back, hip flexors, and gluteal muscles.
- Soft-tissue mobilization around the iliac crest and sacrum.
- Core and hip-strengthening exercises to improve pelvic stability.
- Gait and posture training to reduce repetitive stress on the nerve.
Properly guided exercise can both relieve current symptoms and reduce the chance of recurrence.
3. Medications
Short-term use of:
- Anti-inflammatories (NSAIDs) such as ibuprofen or naproxen
- Topical agents like lidocaine patches or NSAID gels
- In some cases, neuropathic pain medications (e.g., gabapentin, pregabalin—prescription only)
may help dial down pain and nerve sensitivity. Always use medications under medical guidance, especially if you have stomach, kidney, or heart conditions.
4. Cluneal nerve blocks
A cluneal nerve block is both diagnostic and therapeutic:
- Local anesthetic is injected at the suspected entrapment site, often under ultrasound or fluoroscopic guidance.
- Many people experience rapid pain relief, sometimes lasting weeks to months.
- Steroids can be added to decrease local inflammation.
If your pain improves dramatically after a block, but later returns, repeat injections or other minimally invasive options may be considered.
5. Radiofrequency ablation (RFA)
For persistent cluneal nerve pain that responds to nerve blocks but keeps coming back, radiofrequency ablation may be considered:
- A needle is guided to the nerve under imaging.
- Heat energy is used to disrupt pain signal transmission.
- Relief can last several months to over a year in some cases.
This is typically performed by a pain management or interventional spine specialist.
6. Surgical decompression (for select cases)
If conservative measures fail and diagnostic blocks clearly implicate the cluneal nerve, surgical decompression might be an option:
- A small incision is made over the affected area.
- Scar tissue or tight fascial bands compressing the nerve are released.
- The goal is to free the nerve and prevent future entrapment.
Surgery is generally reserved for severe, persistent cases and should be discussed with a surgeon experienced in peripheral nerve procedures.
Self‑care strategies to support long‑term relief
Alongside medical treatments, these self‑care steps can support healing and reduce flare‑ups:
- Maintain healthy weight to reduce mechanical load on the pelvis and lower back.
- Stay active, but paced—frequent short walks, gentle stretching, and avoiding sudden spikes in training volume.
- Use heat or ice:
- Ice during acute flare-ups (10–15 minutes at a time).
- Heat to relax tight muscles around the pelvis.
- Prioritize good sleep—nerve-related pain often worsens with poor rest and stress.
Quick reference: signs your pain may be cluneal nerve–related
You may be dealing with cluneal nerve pain if:
- Pain is focused along the top rim of the pelvis or upper buttock.
- Pressing a very specific spot there reproduces your typical pain.
- Sitting on hard surfaces or having something in your back pocket worsens symptoms.
- Imaging for your spine and hips is “normal” or doesn’t match how much it hurts.
- A local nerve block in that area gives strong temporary relief.
If this sounds familiar, bringing up the cluneal nerve specifically with your doctor or pain specialist can help steer the evaluation in the right direction.
FAQ about cluneal nerve pain
1. What is cluneal nerve entrapment, and how is it different from sciatica?
Cluneal nerve entrapment occurs when one of the cluneal nerve branches is compressed or irritated as it crosses the pelvis or sacrum. It causes localized low back or buttock pain and sometimes tingling or burning in that region. Sciatica usually involves compression of the sciatic nerve from the spine (e.g., a disc herniation) and typically sends pain, numbness, or weakness down the leg, often below the knee. Cluneal neuralgia is more superficial and more localized.
2. Can cluneal nerve damage be permanent?
Most cluneal nerve problems are due to irritation or entrapment, not complete nerve damage. With proper diagnosis, activity changes, and targeted treatments (like nerve blocks or physical therapy), many people experience significant and lasting improvement. Long‑standing, untreated compression can sometimes lead to chronic sensitivity, but true irreversible cluneal nerve damage is less common than persistent inflammation and entrapment.
3. How do you treat superior cluneal nerve pain at home?
For mild to moderate superior cluneal nerve pain, home management can include avoiding hard chairs, using cushions, stopping the habit of sitting on a wallet, gentle stretching of the lower back and hips, anti-inflammatory medication (if safe for you), and heat or ice for comfort. However, if pain persists beyond a few weeks, interferes with walking, work, or sleep, or if you’re not sure of the diagnosis, it’s important to see a clinician to discuss targeted options such as a superior cluneal nerve block.
Take the next step toward real relief
If you’ve been living with unexplained low back or buttock pain, normal imaging, and only partial relief from standard treatments, it may be time to consider the cluneal nerve as a missing piece of the puzzle. Ask your primary care provider, physiatrist, pain specialist, or spine doctor whether cluneal nerve entrapment could be contributing to your symptoms—and whether a focused exam or diagnostic nerve block is appropriate.
You don’t have to accept ongoing “mystery” back pain as your new normal. With the right diagnosis and a targeted plan, cluneal nerve pain is often treatable. Reach out to a qualified professional, share what you’ve learned here, and take a clear, informed step toward lasting relief.