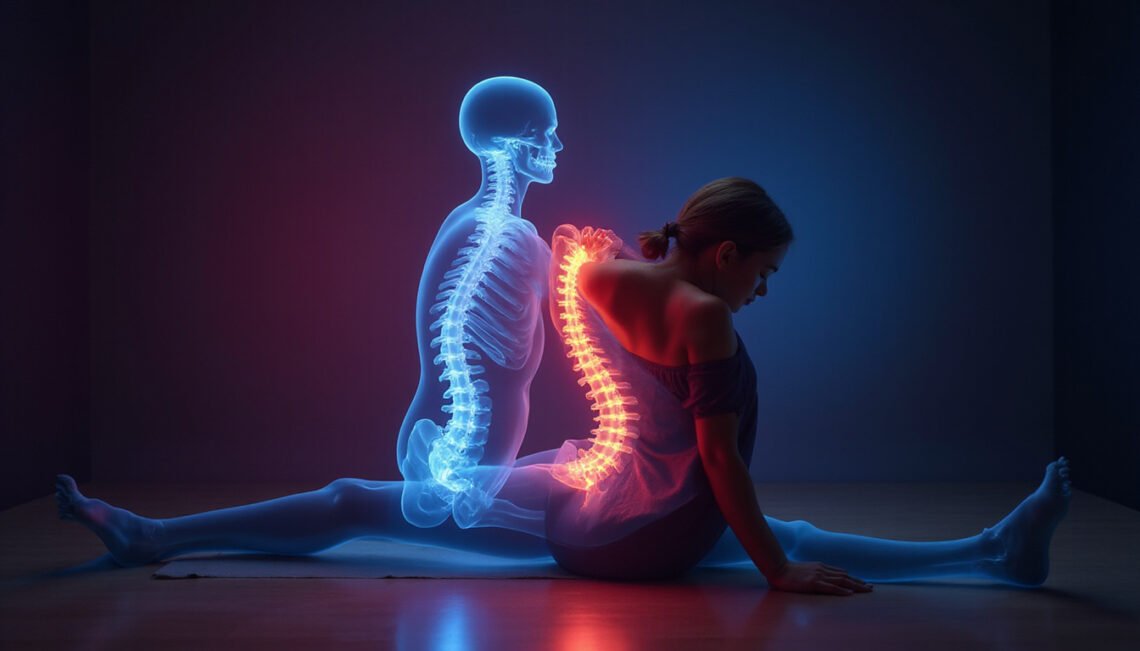
Ankylosing Spondylitis: Breakthrough Strategies To Relieve Pain And Stiffness
Ankylosing spondylitis is a chronic inflammatory arthritis that primarily affects the spine and sacroiliac joints, leading to pain, stiffness, and reduced mobility. While the condition can feel overwhelming, there have been major advances in diagnosis, treatment, and self-management over the past decade. Today, many people with ankylosing spondylitis live active, fulfilling lives by combining medical therapies with targeted lifestyle strategies.
This guide explains what’s happening in your body, the newest evidence-based treatments, and practical, day‑to‑day tactics to reduce pain and stiffness.
Understanding Ankylosing Spondylitis: What’s Really Going On?
Ankylosing spondylitis (AS) is a type of axial spondyloarthritis—a group of inflammatory diseases that mainly affect the spine and pelvis. It’s considered an autoimmune or “auto‑inflammatory” condition: your immune system mistakenly attacks healthy tissue, especially at the points where ligaments and tendons attach to bone (called entheses).
Over time, chronic inflammation can:
- Cause pain and stiffness, especially in the lower back and hips
- Lead to new bone formation and fusion of the spine (ankylosis)
- Reduce flexibility and chest expansion
- Affect other areas (eyes, hips, shoulders, heels, sometimes the gut or skin)
AS usually begins in teens or young adults and is more common in people who carry the HLA‑B27 gene, though not everyone with the gene develops the disease (source: Arthritis Foundation).
Recognizing the pattern of symptoms early is crucial, because timely treatment can slow progression and preserve mobility.
Classic Symptoms: When Pain and Stiffness Are a Warning Sign
Back pain is common, but the back pain of ankylosing spondylitis has some distinct features. It is more likely to be inflammatory rather than mechanical.
Common signs and symptoms include:
- Persistent low back or buttock pain lasting more than three months
- Morning stiffness that lasts 30 minutes or more
- Pain that improves with movement and worsens with rest
- Night pain that can wake you from sleep, especially in the second half of the night
- Reduced flexibility in the spine and neck over time
- Limited chest expansion, making deep breaths uncomfortable
- Fatigue, which can be significant
Some people also experience:
- Eye inflammation (iritis/uveitis): red, painful, light‑sensitive eyes
- Peripheral joint pain (hips, shoulders, knees)
- Heel pain at the Achilles tendon or plantar fascia
- Gut symptoms if inflammatory bowel disease is present
If you have this pattern, especially if you’re under 45 and symptoms have lasted more than a few months, it’s important to see a rheumatologist for evaluation.
Diagnosis: How Doctors Confirm Ankylosing Spondylitis
Diagnosing ankylosing spondylitis combines clinical assessment, imaging, and lab work.
Your rheumatologist will typically:
- Take a detailed history (when symptoms started, what improves/worsens them)
- Examine your spine, hips, chest expansion, and posture
- Order imaging:
- X‑rays of the sacroiliac joints and spine (to look for structural changes)
- MRI, which can detect inflammation before X‑rays change
- Run blood tests:
- Inflammatory markers like ESR or CRP (may be elevated)
- HLA‑B27 gene test (supportive, but not definitive)
- Labs to rule out other causes of back pain
Early or “non‑radiographic axial spondyloarthritis” can exist before X‑ray changes appear, so a normal X‑ray does not necessarily rule out AS. Continued follow‑up is important if symptoms suggest axial spondyloarthritis.
Breakthrough Medical Treatments: What’s New and What Works
The greatest breakthroughs in ankylosing spondylitis management have come from targeted biologic and small‑molecule therapies that directly interrupt key inflammatory pathways.
1. NSAIDs: First‑Line Relief for Pain and Stiffness
Nonsteroidal anti‑inflammatory drugs (NSAIDs) remain the frontline treatment:
- Examples: ibuprofen, naproxen, diclofenac, celecoxib
- Benefits: reduce pain, stiffness, and inflammation; improve function
- Best used under medical supervision due to potential stomach, kidney, and cardiovascular side effects with long‑term use
For some people, consistent NSAID use significantly improves symptoms and quality of life.
2. Biologic Therapies: Targeting TNF and IL‑17
Biologic medications have transformed outcomes for many patients with ankylosing spondylitis.
TNF inhibitors (TNFi) block tumor necrosis factor‑alpha, a key inflammatory molecule:
- Drugs include adalimumab, etanercept, infliximab, golimumab, certolizumab
- Often used when NSAIDs are inadequate
- Can dramatically reduce pain and stiffness, improve function, and may slow structural damage in some patients
IL‑17 inhibitors target interleukin‑17, another major inflammatory pathway:
- Drugs include secukinumab and ixekizumab
- A strong option for people who don’t respond well to or can’t take TNF inhibitors
- Also useful for those with overlapping conditions like psoriasis
These biologics are usually given by injection or infusion. Your rheumatologist will monitor for infections and other rare side effects.
3. Newer Targeted Oral Treatments
A newer class of drugs, JAK inhibitors (e.g., upadacitinib), are small‑molecule pills that interfere with signaling pathways used by several inflammatory cytokines.
For some people, they offer an effective, convenient alternative to injectable biologics. They are newer in ankylosing spondylitis and require lab monitoring due to potential side effects such as elevated cholesterol or increased infection risk.
4. Why Early and Aggressive Treatment Matters
Early initiation of effective anti‑inflammatory therapy can:
- Significantly reduce pain and morning stiffness
- Maintain spinal mobility and posture
- Lower the risk of long‑term complications, like severe spinal fusion or hip damage
- Improve fatigue, mood, and overall quality of life
Modern guidelines encourage a treat‑to‑target approach: working with your rheumatologist to achieve low disease activity or remission, then adjusting treatment as needed to stay there.
Movement as Medicine: Exercise Strategies That Really Help
While medication controls inflammation, movement is the most powerful tool you personally control to preserve function and reduce stiffness.
Daily Stretching and Mobility
Gentle, regular stretching keeps your spine and surrounding muscles flexible:
- Focus on the spine, hips, hamstrings, and chest
- Aim for 10–20 minutes every day, even on low‑pain days
- Move slowly, avoid bouncing, and stay within a comfortable range
Physical therapists with experience in ankylosing spondylitis can design a custom program.
Posture and Extension Exercises
Because AS tends to pull the spine forward into a bent posture, posture training and extension (backward‑bending) exercises are key.
Useful strategies include:
- Wall posture checks: standing against a wall with heels, buttocks, shoulders, and back of head as close to the wall as comfortable
- Gentle back‑extension exercises on the floor or over a therapy ball
- Strengthening the upper back and gluteal muscles to support upright posture
Low‑Impact Cardio
Cardiovascular exercise improves overall fitness, mood, and spinal mobility:
- Swimming and water aerobics
- Walking or using an elliptical
- Cycling, if tolerated and posture is monitored
Aim for a mix of mobility, strength, and aerobic activity most days of the week, adjusted to your capabilities and pain levels.

Lifestyle Tweaks That Reduce Pain and Stiffness
Medications and exercise are pillars of treatment, but daily habits also influence inflammation, comfort, and function.
Sleep, Mattresses, and Pillows
Quality sleep helps manage pain and fatigue:
- A medium‑firm mattress often supports the spine best
- Avoid very high pillows that push the head forward; consider a thin or contour pillow
- Try to sleep on your back or side rather than on your stomach, to protect the neck and lower back
Morning stiffness often eases with a warm shower and gentle stretching before you start the day.
Heat, Cold, and Physical Modalities
- Heat (warm showers, heating pads) relaxes tight muscles and eases stiffness
- Cold packs on inflamed joints can reduce swelling and pain
- Some people benefit from TENS (transcutaneous electrical nerve stimulation) units, massage, or acupuncture as complementary options
Always avoid applying extreme temperatures directly to the skin.
Nutrition and Body Weight
There is no single “ankylosing spondylitis diet,” but certain principles can help:
- Emphasize anti‑inflammatory foods: fruits, vegetables, whole grains, nuts, seeds, olive oil, and fatty fish
- Limit highly processed foods, excess sugar, and trans fats
- Maintain a healthy weight to reduce stress on the hips and spine
For some individuals with overlapping gut issues, tailored diets (e.g., low‑FODMAP for IBS) may be useful under professional guidance.
Smoking and Alcohol
- Smoking is strongly associated with more severe ankylosing spondylitis, worse lung function, and increased structural damage. Stopping smoking is one of the most impactful changes you can make.
- Alcohol in moderation is usually acceptable, but heavy use can worsen sleep, interact with medications, and increase fall risk.
Living Well With Ankylosing Spondylitis: Mind, Work, and Relationships
Chronic conditions affect more than just the body. Addressing emotional and social aspects can reduce stress and improve quality of life.
Managing Stress and Mental Health
Chronic pain and fatigue increase the risk of anxiety and depression. Helpful strategies include:
- Cognitive behavioral therapy (CBT) or other counseling
- Relaxation practices (deep breathing, mindfulness, gentle yoga adapted for AS)
- Planning regular enjoyable activities and social connection
Let your healthcare team know if mood changes, sleep problems, or stress feel overwhelming—mental health support is part of good ankylosing spondylitis care.
Work, Ergonomics, and Daily Tasks
Small adjustments in your environment can reduce strain:
- Use an adjustable chair with lumbar support
- Position screens at eye level to avoid constant neck bending
- Take short movement breaks every 30–60 minutes
- Consider ergonomic keyboards or standing desks if helpful
Occupational therapists can suggest modifications and devices to make daily tasks more comfortable and safe.
Building a Support Network
Connecting with others who understand ankylosing spondylitis can provide practical tips and emotional support. Options include:
- Local or online support groups
- Patient organizations focused on spondyloarthritis
- Peer mentors or community forums
Sharing experiences can make it easier to navigate medication decisions, flares, and life transitions.
Practical Daily Checklist for Managing Ankylosing Spondylitis
You don’t have to do everything at once. Starting with a simple routine can make a big difference. Consider this daily framework and adapt it with your rheumatologist and therapist:
- Take prescribed medications as directed.
- Spend 10–20 minutes on stretching and posture exercises.
- Incorporate at least 20–30 minutes of gentle movement (walk, swim, cycle).
- Use heat in the morning or before exercise to loosen stiffness.
- Take short posture/movement breaks if you sit or stand for long periods.
- Prioritize 7–9 hours of sleep with good sleep hygiene.
- Eat mostly whole, minimally processed foods and stay well‑hydrated.
- Check in with your mood; use relaxation techniques when stressed.
FAQ: Common Questions About Ankylosing Spondylitis
1. What is the difference between ankylosing spondylitis and axial spondyloarthritis?
Axial spondyloarthritis (axSpA) is an umbrella term for inflammatory arthritis affecting the spine and sacroiliac joints. Ankylosing spondylitis is a form of axSpA where structural changes are visible on X‑rays (such as sacroiliitis and new bone formation). Non‑radiographic axial spondyloarthritis has similar symptoms but lacks those X‑ray changes; both are treated in similar ways.
2. Can ankylosing spondylitis be cured or go into remission?
There is currently no cure for ankylosing spondylitis, but many people achieve low disease activity or remission with modern treatments. This means minimal pain and stiffness, good function, and little to no ongoing inflammation. Early diagnosis, appropriate medication, exercise, and healthy lifestyle choices greatly increase the chance of long‑term control.
3. What are the best exercises for ankylosing spondylitis back pain?
The best exercise program for ankylosing spondylitis back pain usually includes:
- Daily stretching for the spine, hips, and hamstrings
- Posture and extension exercises to counter forward bending
- Low‑impact cardio like swimming, walking, or cycling
- Strength training for core and upper back muscles
Working with a physical therapist experienced in spondyloarthritis ensures that movements are safe and tailored to your stage of disease.
Take the Next Step Toward Better Control of Ankylosing Spondylitis
Living with ankylosing spondylitis does not mean surrendering to constant pain and stiffness. With today’s targeted treatments, smart movement strategies, and supportive lifestyle changes, it’s possible to protect your spine, maintain independence, and stay active.
If your back pain or stiffness has been brushed off as “just getting older” or “a pulled muscle” but hasn’t improved, schedule an appointment with a rheumatologist and ask specifically about axial spondyloarthritis. If you already have a diagnosis, use this information to revisit your treatment plan: Are your symptoms truly under control? Are you getting the most from exercise, posture work, and sleep?
The sooner you act, the more of your mobility and quality of life you can preserve. Reach out to a specialist, consider joining a support community, and start implementing one or two new strategies this week. Small, consistent steps can add up to powerful relief from ankylosing spondylitis pain and stiffness.