Minimally Invasive Surgery Breakthroughs: Faster Recovery, Smaller Scars
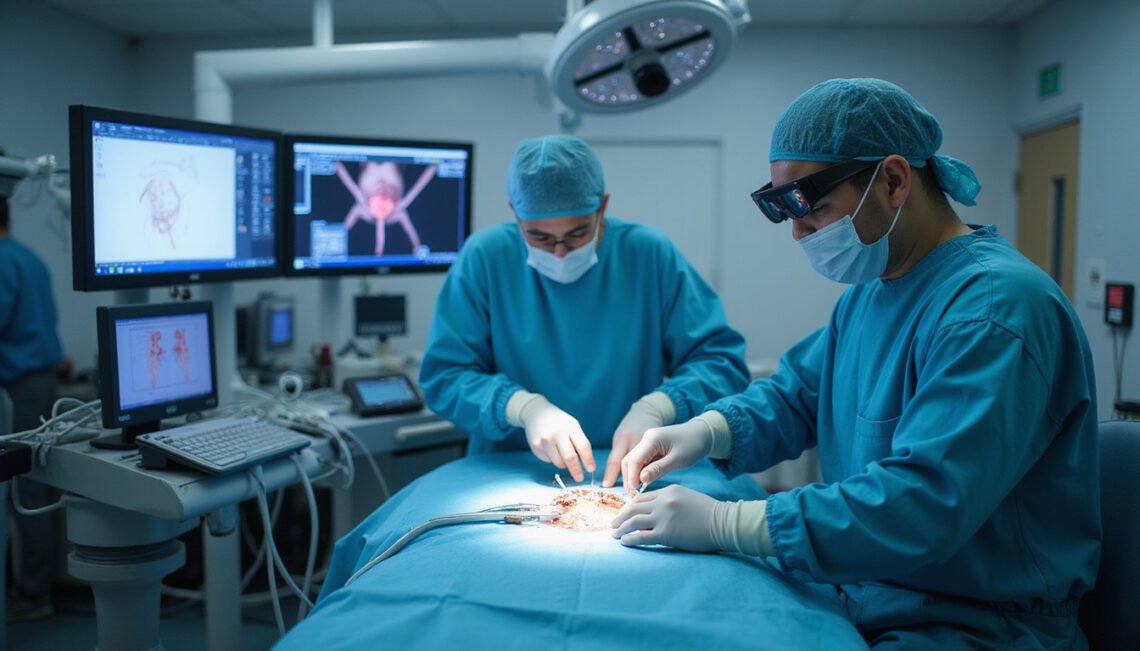
Minimally invasive surgery has transformed how we think about operations, recovery, and even hospital stays. Instead of large incisions, long scars, and weeks in bed, many patients today go home the same day with only a few tiny marks on the skin. Thanks to rapid breakthroughs in technology and technique, minimally invasive surgery now reaches more body systems, treats more conditions, and delivers better outcomes than ever before.
This guide explains what minimally invasive surgery is, how it works, recent innovations, who qualifies, and what you can realistically expect before and after your procedure.
What Is Minimally Invasive Surgery?
Minimally invasive surgery (MIS) is an umbrella term for surgical techniques that use smaller incisions and specialized instruments to minimize damage to healthy tissue. Instead of opening up a large area of the body, surgeons work through tiny “ports” using cameras and long, thin tools.
Common types include:
- Laparoscopic surgery – Uses a thin camera (laparoscope) inserted through small incisions, often in the abdomen.
- Robotic-assisted surgery – Surgeon controls robotic arms from a console, enhancing precision and range of motion.
- Endoscopic surgery – Uses flexible cameras inserted through natural openings (mouth, nose, anus, urethra) rather than external incisions.
- Percutaneous procedures – Needle- or catheter-based techniques, often guided by imaging (X-ray, CT, ultrasound).
While techniques differ, the goals are the same: less pain, fewer complications, and a faster return to normal life.
Why Minimally Invasive Surgery Is a Breakthrough
Traditional open surgery can still be necessary for some complex or emergency cases, but it often involves a long incision, significant blood loss, and prolonged recovery. Minimally invasive surgery reaches the same internal structures through much smaller entry points, which offers several major advantages:
Smaller Scars and Better Cosmetic Results
With incisions typically ranging from 0.5 to 1.5 centimeters, scarring is usually minimal. Many incisions are hidden in natural skin folds or the belly button. For people concerned about body image, clothing choices, or visible reminders of illness, this is a major benefit.
Faster Recovery and Shorter Hospital Stays
Because there is less trauma to muscles, skin, and surrounding tissue:
- Pain is usually less intense.
- Mobility returns more quickly.
- Infection risk is lower.
- Many procedures are done as outpatient surgeries.
Studies have repeatedly shown that hospital stays and recovery times are shorter with minimally invasive approaches when they’re appropriate, compared with open surgery (source: National Institutes of Health).
Lower Risk of Complications
Smaller incisions and more precise instruments can lower the risk of:
- Wound infections
- Excessive blood loss
- Postoperative hernias
- Adhesions (internal scar tissue)
- Breathing problems related to prolonged bed rest
That said, risk is never zero. The key is to match each patient and condition with the right surgical method.
Key Technologies Driving New Breakthroughs
The story of minimally invasive surgery is really a story of technology meeting surgical skill. Several innovations have driven the latest wave of breakthroughs.
High-Definition and 3D Imaging
Early laparoscopes gave surgeons a limited, grainy 2D view. Modern systems offer:
- High-definition video for detailed visualization
- 3D depth perception that mimics natural human vision
- Magnification that can make tiny structures easier to see than in open surgery
These upgrades make it possible to perform complex, delicate operations safely with small incisions.
Robotic-Assisted Surgical Systems
Robotic surgery doesn’t mean a robot operates autonomously. Instead, surgeons sit at a console and control robotic arms that:
- Filter out hand tremors
- Allow more degrees of motion than the human wrist
- Operate in very tight spaces
Robotic-assisted minimally invasive surgery is now common in:
- Prostate and kidney surgery
- Hysterectomies and other gynecologic procedures
- Certain colorectal and thoracic operations
Advanced Energy Devices and Staplers
Modern MIS uses sophisticated tools that can:
- Seal blood vessels with heat or ultrasonic energy
- Cut and staple tissue in one motion
- Reduce bleeding and the need for sutures
These instruments help keep operations efficient and safe, even through tiny ports.
Image-Guided and Navigation Systems
In neurosurgery, orthopedics, and interventional radiology, surgeons now use real-time imaging and navigation systems similar to GPS. These systems allow them to:
- Target tumors or lesions with high precision
- Avoid critical blood vessels and nerves
- Reduce damage to surrounding healthy tissue
Such image-guided minimally invasive approaches are revolutionizing procedures like spine stabilization, brain tumor biopsy, and joint repair.

Common Procedures Now Done Minimally Invasively
Minimally invasive surgery has spread across almost every specialty. Many operations that once required large incisions can now be done with small ports or scopes.
Abdominal and Digestive Surgeries
- Gallbladder removal (cholecystectomy)
- Appendectomy
- Hernia repair
- Anti-reflux surgery (for GERD)
- Bariatric (weight loss) surgery
- Parts of colon and rectal surgery
Gynecologic and Urologic Surgeries
- Hysterectomy
- Fibroid removal (myomectomy)
- Endometriosis resection
- Prostatectomy
- Kidney surgeries (partial or total nephrectomy)
Orthopedic and Spine Procedures
- Arthroscopic surgery for knees, shoulders, hips
- Certain spine decompressions and fusions
- Repair of tendons and ligaments
Heart and Lung Procedures
- Video-assisted thoracoscopic surgery (VATS) for lung nodules
- Minimally invasive valve repair or replacement
- Catheter-based procedures for blocked arteries
The list continues to grow as tools and techniques improve.
What to Expect Before, During, and After MIS
Understanding the process can reduce anxiety and help you prepare.
Before Surgery
You’ll typically go through:
- A detailed consultation and physical exam
- Imaging tests (e.g., ultrasound, CT, MRI)
- Labs to check blood counts and organ function
- Review of medications and allergies
Your surgeon will explain:
- Why minimally invasive surgery is recommended
- Alternatives (including open surgery)
- Potential risks and benefits
- Recovery timeline
This is the time to ask every question on your mind, from scar size to when you can return to work.
During Surgery
While procedures vary, most follow a similar pattern:
- Anesthesia – You’re usually under general anesthesia, meaning you’re asleep and pain-free.
- Small incisions – The surgeon makes several tiny cuts for the camera and instruments.
- Visualization – The camera sends a live feed to video monitors.
- Operation – The surgeon performs the necessary steps: removing diseased tissue, repairing structures, or reconstructing anatomy.
- Closure – Instruments are removed, and incisions are closed with sutures, staples, or surgical glue.
Operating time may be similar to or slightly longer than open surgery, especially for complex cases, but overall recovery is often much shorter.
After Surgery
Postoperative advantages of minimally invasive surgery often include:
- Less pain and reduced need for strong narcotics
- Earlier walking and breathing exercises
- Faster return of bowel function
- Quicker discharge (sometimes same day)
Your care team will give you specific instructions about:
- Activity limits
- Showering and caring for incisions
- Signs of complications (e.g., fever, increasing pain, redness)
- Follow-up appointments
Who Is a Good Candidate for Minimally Invasive Surgery?
Not everyone is automatically a candidate, but many are. Surgeons consider:
- Type and stage of the condition – Some advanced cancers, extensive infections, or emergencies may still need open surgery.
- Overall health – Heart and lung disease, obesity, or previous surgeries can affect the plan, but they don’t always exclude MIS.
- Anatomy and prior operations – Scar tissue from prior surgeries can make MIS more challenging, but not impossible.
- Surgeon and facility expertise – Availability of specific equipment and trained teams matters.
A key principle: the safest, most effective approach for your condition should come first—whether that’s minimally invasive, open, or a hybrid. Ask your surgeon directly why they recommend a certain approach and whether a minimally invasive option is appropriate.
Preparing Yourself for a Smoother Recovery
You can play an active role in making the most of minimally invasive surgery. Preparation and aftercare matter.
Consider these steps:
-
Optimize health beforehand
- Stop smoking if possible.
- Control blood pressure, diabetes, and other chronic conditions.
- Improve nutrition and hydration.
-
Follow fasting and medication instructions
- Don’t eat or drink when told not to.
- Ask which medications to take or hold on surgery day.
-
Arrange support at home
- Have someone drive you home.
- Prepare easy meals and a comfortable resting area.
-
Move early, but safely
- Follow your team’s advice on walking and gentle activity.
- Movement helps prevent blood clots and speeds healing.
-
Protect your incisions
- Keep them clean and dry as directed.
- Avoid heavy lifting until cleared.
Being proactive can help you fully benefit from the faster recovery and smaller scars that minimally invasive surgery offers.
Frequently Asked Questions About Minimally Invasive Surgery
Is minimally invasive surgery safer than traditional open surgery?
For many planned procedures in appropriate patients, minimally invasive surgery is at least as safe as open surgery and often carries a lower risk of certain complications, like wound infections and blood loss. However, “safer” depends on your specific condition, the surgeon’s experience, and your overall health. Your surgeon can compare the risks and benefits of minimally invasive vs. open approaches for your situation.
How long does it take to recover from a minimally invasive procedure?
Recovery times vary by surgery type and individual factors, but many people:
- Go home the same day or within 24–48 hours.
- Return to light activities in a few days.
- Resume work in 1–3 weeks for many common procedures.
More complex minimally invasive operations, such as major cancer surgeries, may still require several weeks of recovery, but typically less than similar open operations.
Are all surgeries now performed using minimally invasive techniques?
No. While the use of minimally invasive and laparoscopic surgery continues to expand, some operations still require an open approach. Reasons include:
- Emergency situations with internal bleeding or infection
- Very large or invasive tumors
- Complex anatomy or extensive scar tissue
- Lack of appropriate MIS equipment or expertise
In some cases, a minimally invasive surgery must be converted to open surgery mid-procedure for safety. This is not a failure; it’s a decision to prioritize the best outcome.
Taking the Next Step
If you’ve been told you need an operation—or you’re exploring treatment options for a condition that might require surgery—asking about minimally invasive surgery is a smart, proactive step. A brief conversation with a qualified surgeon can clarify:
- Whether you’re a good candidate
- The expected benefits and risks
- How your recovery is likely to look
- What experience your surgeon and hospital have with the specific procedure
You deserve clear answers and a treatment plan that fits your life, not just your diagnosis. Reach out to a board-certified surgeon or a high-quality surgical center, schedule a consultation, and use this information as a framework for your questions. With the right team and the right approach, you can make the most of today’s minimally invasive surgery breakthroughs—and move toward healing with faster recovery, smaller scars, and greater confidence in the road ahead.