Peroneal Nerve Injury: 9 Simple Fixes to Restore Foot Function
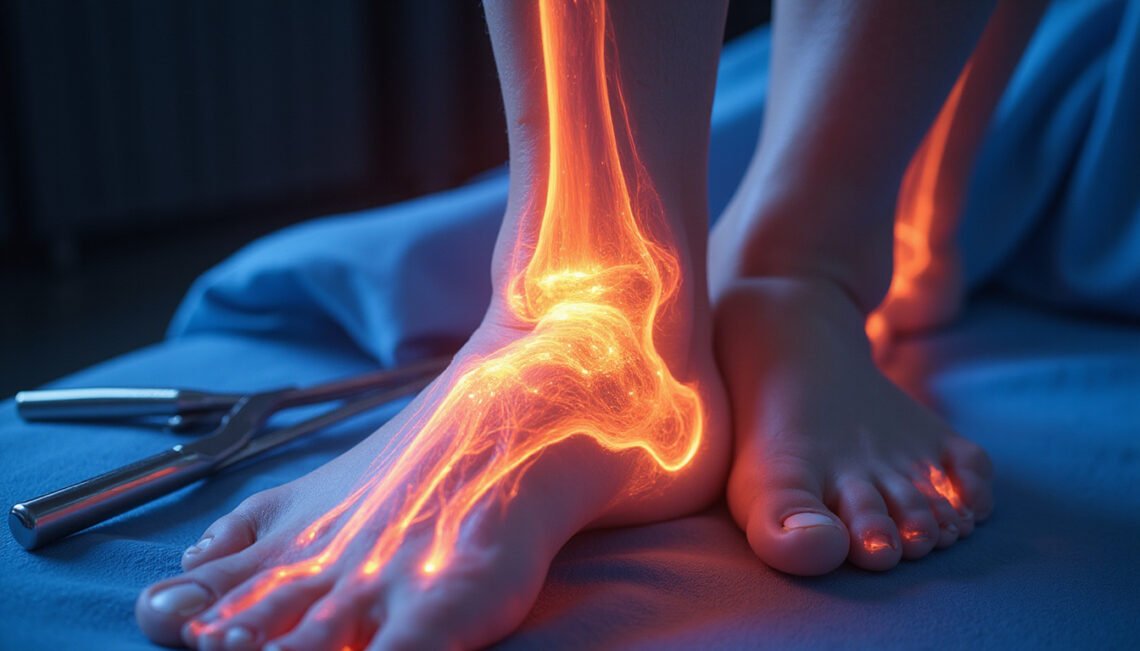
The peroneal nerve (also called the common fibular nerve) plays a crucial role in lifting your foot and toes and turning the foot outwards. When it’s injured or compressed, walking, balance, and even standing can become difficult. If you’re dealing with foot drop, numbness along the outer leg, or weakness in your ankle, understanding peroneal nerve injury and how to help it heal is essential.
Below are nine practical, simple strategies you can start using—often at home—to restore foot function and support long‑term nerve health.
Understanding the Peroneal Nerve and Foot Drop
The peroneal nerve branches from the sciatic nerve, wrapping around the outside of the knee (near the head of the fibula) and traveling down the outer lower leg. It controls:
- Dorsiflexion: lifting your foot and toes
- Eversion: turning your foot outward
- Sensation: along the outer lower leg and top of the foot
Common signs of peroneal nerve injury include:
- Foot drop (difficulty lifting the front of the foot)
- Toe drag while walking
- Numbness or tingling on the top of the foot or outer leg
- Weakness when lifting the toes or ankle
- Tripping or slapping the foot down when walking
Injuries can result from trauma (knee or fibula fracture), surgery around the knee/hip, prolonged crossing of the legs, tight casts or braces, or even rapid weight loss affecting padding around the nerve.
1. Identify and Remove Pressure on the Nerve
The first “fix” is often the most important: stop whatever is irritating the peroneal nerve.
Common sources of compression:
- Habitual leg crossing (especially right over left or vice versa for hours)
- Tight boots, knee braces, or casts
- Squatting or kneeling for long periods (gardening, flooring work, mechanics)
- Prolonged bed rest with the outer knee resting against a hard surface
What to do:
- Avoid leg crossing for several weeks and see if symptoms improve.
- Loosen or replace restrictive footwear or braces.
- Use a soft pillow under the outer knee when lying on your side.
- If you wear a knee brace, ask your provider or physical therapist to check its fit.
For many mild peroneal nerve compressions, simply removing mechanical pressure allows the nerve to begin recovering.
2. Support Walking with an Ankle-Foot Orthosis (AFO)
When the peroneal nerve is weak, foot drop can cause dangerous trips and falls. An ankle‑foot orthosis (AFO) is a lightweight brace that holds your ankle and foot in a safer, more neutral position.
Benefits of an AFO:
- Prevents toe drag and reduces tripping
- Promotes a more normal walking pattern
- Takes strain off overstressed muscles
- Helps protect joints while the nerve heals
Modern AFOs can be slim and fit into many regular shoes. A physical therapist or orthotist can recommend the style best for your level of weakness and your lifestyle (work, sport, daily walking).
3. Start Gentle Ankle and Toe Activation Exercises
Early, gentle movement helps maintain joint flexibility and can support nerve recovery by improving blood flow to the area. Never force a movement that causes sharp pain; work within your current ability.
Basic activation exercises
Try these 1–2 times daily, as tolerated:
-
Assisted dorsiflexion:
- Sit with your leg outstretched.
- Loop a towel around the ball of your foot.
- Use your hands to gently pull your foot toward you, then slowly release.
- Repeat 10–15 times.
-
Toe taps (if possible):
- Sitting with your heel on the floor, try lifting your toes up and down.
- Even small movements are helpful; quality over range.
- Do 2 sets of 10–15 reps.
-
Ankle circles:
- Draw circles with your foot in both directions, keeping the movement within comfort.
- 10 circles each way, 1–2 sets.
These movements maintain mobility in the ankle and foot, which is important while waiting for the peroneal nerve to regenerate.
4. Strengthen the Muscles that Lift and Stabilize the Foot
As function returns, targeted strengthening helps restore power and control. Always follow your healthcare provider’s or physical therapist’s clearance before starting more advanced exercises.
Simple strengthening ideas
-
Resisted dorsiflexion with band
- Sit with your leg out straight.
- Attach a resistance band around the ball of your foot and hold the ends with your hands.
- Slowly pull your toes toward your shin against the band, then return.
- 2–3 sets of 10–15 reps.
-
Side‑lying eversion
- Lie on your side, affected leg on top.
- Keep your knee straight and slowly turn your foot outward (sole away from your other leg).
- Hold 2–3 seconds, then relax.
- 2 sets of 10–15 reps.
-
Heel walking (only if safe)
- In a hallway or near a support, gently try to walk a short distance on your heels with toes up.
- If your foot drops too much or you feel unsteady, skip this and return to bracing.
Consistency matters more than intensity. Progress should be gradual and guided by a professional where possible.
5. Protect Sensation and Skin Health
The peroneal nerve also carries sensory information. If you have numbness or altered sensation on the outer leg or top of the foot, you may be at higher risk of skin breakdown or injury because you can’t feel irritation as well.
Protective strategies:
- Inspect your foot and outer shin daily for redness, blisters, cuts, or pressure marks.
- Choose well‑fitting shoes with enough room in the toe box; avoid seams that rub.
- Wear moisture‑wicking socks to reduce friction.
- Avoid walking barefoot on hot surfaces (sand, pavement) or in unfamiliar areas.
This approach is similar to foot‑care principles used in diabetic neuropathy and can prevent avoidable complications (source: American Academy of Neurology).
6. Use Posture and Ergonomics to Reduce Nerve Stress
The peroneal nerve is particularly vulnerable around the outside of the knee. Simple postural adjustments can relieve ongoing low‑grade pressure.
Check and adjust these habits:
-
Sitting posture:
- Keep both feet flat when possible.
- Avoid sitting on your heels or tucking your legs underneath you.
- Use a footrest if your chair is high.
-
Work tasks involving kneeling/squatting:
- Use kneeling pads or a small stool.
- Take micro‑breaks every 15–20 minutes to stand and move.
-
Sleep position:
- If you sleep on your side, place a soft pillow between your knees and under the outer side of the upper leg to reduce pressure on the nerve.
Small postural changes, repeated many hours a day, can significantly affect how much mechanical stress the peroneal nerve experiences.
7. Consider Physical Therapy for Gait Retraining
When the peroneal nerve is impaired, your body automatically compensates with altered movement patterns. Over time, this can strain hips, knees, and the low back.
A physical therapist can:
- Analyze your gait (walking pattern)
- Recommend or fit an AFO or other brace
- Teach compensatory strategies to reduce tripping risk:
- Slightly higher knee lift
- Shorter steps
- Use of walking aids temporarily
- Prescribe progressive exercises to:
- Strengthen supporting muscles (glutes, hamstrings, calves)
- Improve balance and proprioception
- Normalize timing and rhythm of walking
Even a few focused PT sessions can give you a personalized home program and greatly improve walking safety and efficiency.
8. Use Pain and Inflammation Management Wisely
Some peroneal nerve injuries are associated with local inflammation around the knee, fibular head, or surrounding soft tissues.
Possible options (under professional guidance):
- Short‑term use of NSAIDs (e.g., ibuprofen) if appropriate for your health history
- Ice packs over the outer knee (10–15 minutes, with cloth barrier, a few times daily)
- Relative rest from aggravating activities such as deep squatting or prolonged kneeling
- In select cases, your doctor may consider a corticosteroid injection near compressive structures—this must be done carefully, by an experienced clinician, to avoid additional nerve irritation.
Important: Shooting, electric pain, or rapidly worsening weakness should be evaluated promptly. These may signal active nerve compromise that needs urgent attention.
9. Explore Medical and Surgical Options When Needed
Not all peroneal nerve injuries can be resolved with conservative methods. The nature and severity of the injury matter.
When to seek specialist evaluation:
- You cannot lift your foot at all (complete foot drop).
- Symptoms appeared suddenly after trauma or surgery.
- Weakness or numbness is worsening over weeks.
- No meaningful improvement after 3–6 months of conservative care.
A neurologist or orthopedic surgeon may recommend:
- Nerve conduction studies and EMG to assess the location and severity of nerve damage.
- Imaging (MRI, ultrasound) to look for masses, cysts, or structural causes compressing the nerve.
- Surgical decompression if the nerve is trapped or compressed by a structure (e.g., fibrous band, cyst).
- Nerve repair, graft, or transfer in cases of severe traumatic injury.
- Tendon transfer procedures to restore active foot dorsiflexion when nerve recovery is unlikely.
Early diagnosis improves the odds of meaningful recovery. Nerves regenerate slowly—often 1–3 mm per day—so long‑term follow‑up and realistic expectations are important.
How Long Does Peroneal Nerve Recovery Take?
Recovery from a peroneal nerve injury depends on:
- Cause (compression vs cut/tear)
- Severity
- How quickly the cause was removed or treated
- Your overall health (including diabetes, smoking, nutrition)
Mild compressions may improve noticeably in weeks to a few months once pressure is relieved. More severe injuries can take 6–18 months or longer, and some may not fully recover.
During this time, protecting joint alignment (bracing when needed), keeping muscles and joints as strong and mobile as safely possible, and preventing falls are critical.
Quick Summary: 9 Simple Fixes for Peroneal Nerve Injury
To make things easier, here’s a concise list of strategies discussed above:
- Remove pressure on the nerve (avoid leg crossing, tight gear, hard surfaces at the outer knee).
- Use an AFO brace to prevent tripping and support safer walking.
- Do gentle mobility exercises to keep the ankle and toes moving.
- Gradually strengthen dorsiflexion and eversion muscles as they recover.
- Protect skin and sensation on the outer leg and top of the foot.
- Improve posture and ergonomics at work, home, and during sleep.
- See a physical therapist for gait retraining and individualized rehab.
- Manage pain and inflammation sensibly under medical guidance.
- Consult specialists for diagnostics or surgery when symptoms are severe or not improving.
FAQ About Peroneal Nerve Problems
1. How is a peroneal nerve injury diagnosed?
Doctors often start with a physical exam, testing muscle strength, reflexes, and sensation around the leg and foot. To confirm a peroneal nerve neuropathy, they may order nerve conduction studies and EMG to see how well electrical signals travel along the nerve and how muscles respond. Imaging like MRI or ultrasound can help find structural causes such as cysts or compression.
2. Can peroneal nerve damage be reversed?
Many cases of peroneal nerve damage caused by compression or mild trauma can improve—sometimes significantly—if the underlying cause is corrected early. However, if the nerve is severely cut or scarred, full reversal may not be possible, and treatment focuses on maximizing remaining function through bracing, therapy, and sometimes surgery.
3. What is the best treatment for peroneal nerve palsy?
The best treatment for peroneal nerve palsy depends on why it happened and how severe it is. For mild, compression‑related cases, removing pressure, using an AFO, and doing targeted physical therapy can be highly effective. For more severe palsy, specialist care may include nerve decompression or repair, and in long‑standing cases, tendon transfer surgery to restore the ability to lift the foot.
Regaining foot function after a peroneal nerve injury is rarely instant, but meaningful progress is possible with the right plan. Start by removing pressure on the nerve, protecting your foot with proper bracing and footwear, and building a safe, consistent exercise routine. Then, partner with a physical therapist and medical specialist to tailor treatment to your specific situation. Don’t wait for symptoms to “just go away”—take action now to safeguard your mobility, reduce fall risk, and reclaim your independence.