Saddle Anesthesia: Essential Signs, Risks, Treatment, and Recovery Tips
Saddle anesthesia is a red-flag symptom that signals a potential emergency involving the lower spine and nerves. Recognizing saddle anesthesia early—and knowing when to seek urgent medical care—can make the difference between full recovery and permanent disability. This guide explains what it is, how to recognize it, what conditions cause it, treatment options, and practical recovery tips.
What Is Saddle Anesthesia?
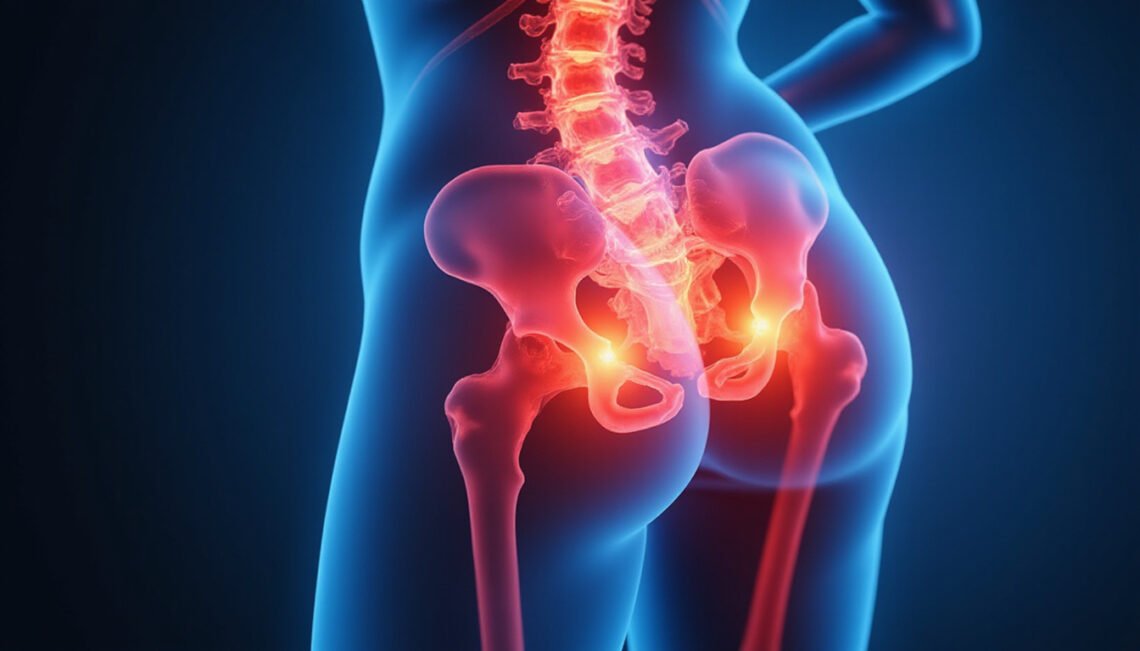
“Saddle anesthesia” refers to numbness, reduced sensation, or altered feeling in the areas of the body that would touch a saddle if you were sitting on a horse. This typically includes:
- Inner thighs
- Buttocks
- Perineum (the area between the genitals and anus)
- Around the anus and sometimes the genital region
It is not a disease itself, but a sign that the nerves serving this region—mainly the sacral nerve roots—are being compressed or damaged. These nerves are responsible for sensation and muscle control in the pelvic floor, bladder, bowel, and some sexual function.
Because these nerve roots are located at the very end of the spinal cord in the lower back, saddle anesthesia is often associated with serious spinal problems, most notably cauda equina syndrome.
Why Saddle Anesthesia Is a Medical Emergency
Saddle anesthesia is considered an emergency warning sign in neurology and spine medicine. It frequently indicates compression of the cauda equina, the bundle of nerve roots at the base of the spinal cord.
If these nerves remain compressed, they can suffer permanent damage, leading to:
- Loss of bladder control (urinary incontinence or retention)
- Bowel incontinence
- Sexual dysfunction
- Weakness or paralysis in the legs
- Chronic pain and numbness
Medical guidelines emphasize that early diagnosis and surgical decompression—often within 24–48 hours of symptom onset—improve the chances of regaining function (source: American Association of Neurological Surgeons). Delays can dramatically worsen long-term outcomes.
If you experience new saddle anesthesia, especially with bladder or bowel changes, it should be treated as an emergency and evaluated immediately in an emergency department.
Key Signs and Symptoms to Watch For
Saddle anesthesia doesn’t always appear alone. It commonly occurs alongside other neurological and spinal symptoms. Watch for the following warning signs:
1. Sensory Changes in the “Saddle” Area
- Numbness, tingling, or “pins and needles” around the inner thighs, buttocks, genitals, and anus
- Decreased or absent sensation when wiping after using the bathroom
- Feeling “cottony,” “dead,” or different when sitting down
- Reduced ability to feel temperature or pain (e.g., water in the shower feels “dull” in that area)
2. Bladder and Bowel Problems
Changes in bladder or bowel function alongside saddle anesthesia are highly concerning. Possible symptoms include:
- Difficulty starting or stopping urination
- Reduced sensation when the bladder is full
- Inability to fully empty the bladder (urinary retention)
- Urine leaking or complete loss of urinary control
- Constipation or loss of bowel control
- Not feeling the urge to have a bowel movement
3. Leg Symptoms and Back Pain
Because the same nerve roots also supply the legs, you may notice:
- Severe low back pain
- Pain radiating down one or both legs (sciatica)
- Weakness in the legs or difficulty walking
- A feeling that the legs are “heavy” or “giving way”
- Loss of reflexes in the knees or ankles
4. Sexual Dysfunction
Saddle anesthesia can affect sexual function, including:
- Numbness in the genitals
- Reduced sexual pleasure or sensation
- Erectile dysfunction or difficulty with arousal and orgasm
If any combination of these symptoms appears suddenly, especially after a back injury or in the setting of known spine disease, seek emergency care right away.
Common Causes of Saddle Anesthesia
Several conditions can compress or damage the nerve roots responsible for sensation in the saddle region. The most common causes include:
1. Cauda Equina Syndrome (CES)
This is the most important and classic cause of saddle anesthesia. Cauda equina syndrome occurs when something compresses the bundle of nerve roots at the lower end of the spinal cord. Causes include:
- A large herniated lumbar disc (often L4/L5 or L5/S1)
- Spinal stenosis (narrowing of the spinal canal)
- Spinal tumors or metastases
- Spinal infections or abscesses
- Spinal trauma or fractures
- Post-surgical complications or hematoma
CES almost always requires urgent neurosurgical evaluation.
2. Severe Lumbar Disc Herniation
Sometimes a large disc herniation produces early or partial saddle anesthesia before full-blown cauda equina syndrome develops. This is still very serious and may progress quickly.
3. Spinal Tumors and Cysts
Growths in the lower spine—such as meningiomas, schwannomas, metastases, or arachnoid cysts—can gradually compress sacral nerve roots. Symptoms may start subtly and worsen over time.
4. Infections and Inflammatory Conditions
- Epidural abscess (a collection of pus around the spinal cord)
- Spinal tuberculosis or osteomyelitis
- Inflammatory disorders such as arachnoiditis
These can irritate or compress the nerves and cause saddle anesthesia alongside systemic symptoms like fever or weight loss.
5. Trauma and Post-Operative Complications
- Falls, car accidents, or sports injuries that damage the lower spine
- Bleeding (hematoma) after spinal or epidural anesthesia
- Post-surgical scarring or hardware complications
Even when the cause seems obvious—such as after a fall—saddle anesthesia always deserves immediate evaluation.
How Doctors Diagnose Saddle Anesthesia and Its Cause
When you present with saddle anesthesia, clinicians move quickly to confirm the diagnosis and locate the source of nerve compression.
1. Detailed Medical History
Your doctor will ask about:
- Onset and progression of numbness
- Back pain and leg symptoms
- Bladder, bowel, and sexual function
- Recent trauma, surgery, infections, or cancers
- Use of blood thinners (increases risk of spinal hematoma)
2. Neurological and Physical Exam
This includes checking:
- Sensation in the saddle area with light touch or pinprick
- Strength and reflexes in the legs
- Anal tone and reflex (important for cauda equina assessment)
- Gait and balance
- Ability to perceive urinary and rectal sensations
3. Imaging Studies
The primary imaging tool is:
- MRI of the lumbar spine – best for visualizing disc herniations, tumors, infections, and nerve compression
In some cases:
- CT scan if MRI is not available or contraindicated
- X-rays to assess bone alignment or fractures (less useful for soft tissue and nerves)
4. Additional Tests
Depending on suspicion:
- Blood tests for infection or inflammation
- Bladder scan to check for retained urine
- Nerve conduction studies in complex or chronic cases
Prompt imaging is crucial; many emergency departments fast-track suspected cauda equina cases for urgent MRI.
Treatment Options for Saddle Anesthesia
The treatment for saddle anesthesia depends on the underlying cause, but in most serious cases the goal is to relieve pressure on the nerves as quickly as possible.
1. Emergency Surgical Decompression
For cauda equina syndrome and other major compressive lesions, surgery is typically the main treatment. Procedures may include:
- Lumbar laminectomy – removing part of the vertebral bone to create space
- Discectomy – removing the herniated portion of a disc
- Tumor or cyst removal
- Drainage of abscess or hematoma
Surgery performed promptly—often within 24–48 hours of onset of bladder, bowel, or saddle sensory changes—offers the best chance to restore function.
2. Treatment of Underlying Conditions
- Antibiotics for spinal infections
- Steroids or other medications for inflammatory conditions
- Radiation or chemotherapy for certain spinal tumors
3. Medical and Supportive Care
- Pain management (non-opioid and opioid medications, as needed)
- Bladder management (catheters, medications to help empty or relax the bladder)
- Bowel regimen to prevent constipation or manage incontinence
Even after the main issue is addressed, symptoms can take weeks or months to improve, and some deficits may be permanent.
Recovery and Rehabilitation: What to Expect
Recovery after saddle anesthesia varies widely. Some people regain nearly full function, while others may live with chronic changes. Factors that influence recovery include:
- How quickly treatment was received
- The severity and duration of nerve compression
- The underlying cause (e.g., trauma vs. tumor vs. herniated disc)
- Your general health and age
Early Recovery Phase (First Few Weeks)
You may experience:
- Gradual return of sensation in the saddle area
- Fluctuations in numbness or tingling
- Ongoing bladder or bowel issues that improve slowly
- Pain and fatigue after surgery
Working closely with your medical team, you’ll likely start physical therapy and possibly occupational therapy to help restore mobility and daily function.
Longer-Term Recovery (Months and Beyond)
Some symptoms can continue to improve for 6–18 months as nerves heal. Others may persist, especially if compression was severe or prolonged. Long-term issues can include:
- Partial numbness or altered sensation
- Mild to moderate weakness in the legs
- Persistent bladder or bowel control problems
- Sexual dysfunction
- Chronic back or nerve pain
Even if full recovery isn’t possible, rehabilitation can significantly improve independence and quality of life.
Practical Tips for Living With or Recovering From Saddle Anesthesia
Beyond medical treatment, certain practical strategies can support recovery and daily functioning. Consider the following:
-
Follow all post-operative and medical instructions closely
- Take medications as prescribed
- Attend all follow-up appointments and imaging checks
-
Prioritize physical therapy
- Focus on core and back strengthening, balance, and gait training
- Learn safe movement techniques to protect your spine
-
Manage bladder and bowel health
- Maintain a regular schedule for bathroom visits
- Use a bladder diary if recommended
- Discuss pelvic floor therapy or continence aids with your team
-
Protect skin in numb areas
- Check the saddle region daily for irritation, pressure sores, or injuries
- Use cushions or special seating if you sit for long periods
-
Address sexual health openly
- Talk with your provider about changes in sensation or function
- Ask about medications, devices, or sexual therapy support
-
Support mental and emotional wellbeing
- Changes in continence or sexual function can be emotionally challenging
- Consider counseling, peer support groups, or online communities
-
Know your limits and pace activity
- Avoid heavy lifting or high-impact sports until cleared
- Gradually build up walking and low-impact exercise
When to Seek Immediate Medical Help
Even during recovery, there are times when urgent evaluation is needed. Contact emergency services or go to the ER if you experience:
- New or worsening saddle anesthesia
- Sudden loss of bladder or bowel control
- New difficulty starting urination
- Rapidly progressing leg weakness or inability to walk
- Severe new back pain after trauma, fall, or injection in the spine
Never ignore new or suddenly worsening neurological symptoms in the lower body.
FAQ: Saddle Anesthesia and Related Concerns
1. What causes numbness in the saddle area besides cauda equina syndrome?
While cauda equina syndrome is the classic cause, saddle anesthesia can also result from severe lumbar disc herniations, spinal tumors, infections, traumatic injuries, or complications after spinal or epidural anesthesia. Rarely, peripheral nerve or pelvic conditions can mimic these symptoms, but any true numbness in the saddle region should be treated as a possible spinal emergency until proven otherwise.
2. Can saddle paresthesia go away on its own?
Mild “saddle paresthesia” (tingling or altered sensation in the saddle area) might fluctuate or temporarily improve, but if it’s due to nerve compression in the spine, waiting is risky. Early imaging and evaluation are crucial. Even if symptoms seem to lessen, underlying nerve damage can progress. Do not assume it will resolve by itself—get urgent medical assessment.
3. How long does it take to recover from saddle anesthesia and cauda equina symptoms?
Recovery time varies. Some patients see noticeable improvement in weeks, while others experience gradual changes over 6–18 months. Sensation in the saddle region, bladder and bowel control, and leg strength may each recover at different speeds. Early decompression surgery tends to improve the odds of better recovery, but some people may still have long-term or permanent deficits.
Take Action Quickly—and Protect Your Long-Term Health
Saddle anesthesia is not a symptom to watch and wait. It is a critical warning sign that the nerves controlling your lower body, bladder, and bowel may be at risk. If you or someone close to you notices new numbness in the saddle area—especially together with changes in urination, bowel movements, or leg strength—seek emergency medical care immediately.
Prompt evaluation, accurate diagnosis, and timely treatment can dramatically improve outcomes and help preserve independence, mobility, and quality of life. If you’ve already been treated for saddle anesthesia, keep working closely with your healthcare and rehabilitation team, ask questions, and advocate for the therapies and support you need to recover as fully as possible.